You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Today in dentistry, minimally invasive tooth extraction followed by immediate implant placement is a frequently used technique to replace compromised teeth.1,2 Recommendations that have been discussed in the literature for obtaining predictable results include avoiding the use of flap releasing,3 minimizing trauma during tooth extraction, placing the implant in a palatal position, and filling the bone-implant gap with bone substitute to preserve the buccal wall.1,2 Adherence to these recommendations combined with the use of Morse-tapered frictional implants should lead to improved biological results with regard to soft- and hard-tissue stability.4 However, even with an optimally appearing pink esthetic, obtaining a global esthetic result over teeth and implants is highly dependent on, among other things, the choice of restorative material.
Along with the advancement of CAD/CAM technologies, new ceramic materials have been introduced to overcome some limitations of metal-ceramic restorations.5 For example, zirconia-based materials are widely used in dental practice because of their good optical and mechanical differentiation properties.6 Allotropic characteristics of zirconia allow this material to exist in different crystalline phases depending on the temperature.7 Yttria-stabilized tetragonal zirconia polycrystal (Y-TZP), which is the most-used zirconia, contains 1 to 3 mol% yttrium oxide to allow it to maintain its tetragonal phase at room temperature and show high fracture strength (>1 GPa) and toughness (>4-6 MPa / m1/2).6 Y-TZP is versatile, ranging in applications from fixed dental prostheses (FDPs), to intracanal posts, to orthodontic brackets, and implants and implant abutments.8,9
Even conventional, or first-generation, zirconia continues to be widely used. It presents some optical limitations, which are mainly related to its white opaque color and reduced transmittance and lack of fluorescence, which are key aspects to recreating natural-appearing restorations.10,11
To enable conventional zirconia to achieve natural shade, fluorescence, and opalescence characteristics, veneering with feldspathic ceramics emerged as an option.12 High rates of veneer chipping, however, are prevalent in bilaminar prostheses, compromising final rehabilitation treatments.13 To overcome this problem and avoid chipping, zirconia monolithic restorations are presently frequently indicated. More recently, high-translucent or third-generation zirconia has been introduced with major modifications in its microstructure for the fabrication of monolithic esthetic restorations. These modifications include smaller particle size, higher density, and the presence of up to 53% cubic zirconia in its composition due to an increase of yttrium oxide (approximately 9.3 wt%/5 mol%).11,14,15
Optical properties of materials are important to enable restorations to match the look of natural teeth; however, achieving consistent esthetic results on different substrates, such as teeth and implants, can be challenging to clinicians.16 The clinical observation of the optical behavior of materials is critical yet not widely presented in the literature. Therefore, the aim of this article is to graphically show the color, fluorescence, opalescence, and transmittance differences among conventional veneered zirconia crowns, high-translucent monolithic zirconia crowns, and minimally veneered high-translucent zirconia crowns on different substrates, namely implant abutments and natural teeth.
Clinical Report
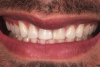
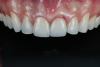
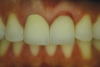
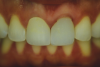
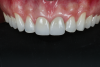
A young man presented concerned about the mobility of his left central incisor and the unpleasant esthetic appearance of both central incisors (Figure 1). After clinical examination and cone-beam computed tomography (CBCT) scanning, a root fracture on the left central incisor was confirmed, indicating its extraction. The right central incisor presented root canal treatment, and because there had been several restorations on the tooth, a total crown was recommended.
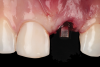
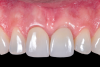
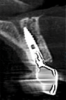
After planning, the dental team opted to place an implant immediately after extracting the fractured left central incisor. Implant osteotomies were prepared according to manufacturer recommendation. A Morse-tapered 3.3 mm x 13 mm frictional implant was installed. A high primary stability of 40 Ncm was obtained, and immediate provisionalization of the implant was performed over a 2.5 mm x 3 mm x 6 mm frictional abutment for cemented restorations (Figure 2). An interim crown was then fabricated and cemented with a temporary cement.
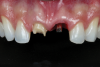
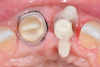
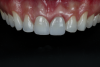
After 3 months, when osseointegration was achieved, the definitive rehabilitation planning began (Figure 3). On the right central incisor, a fiber post was cemented and a build-up with composite resin was performed to facilitate placement of a complete ceramic crown. Upon completion of tooth preparation, polishing, and finishing, a vinyl polysiloxane impression was made of the implant abutment and tooth (Figure 4). The cast was scanned, and three pairs of crowns were fabricated using different materials and techniques: conventional zirconia veneered with feldspathic ceramic (Figure 5 through Figure 7), high-translucent monolithic zirconia (Figure 8 through Figure 10), and high-translucent monolithic zirconia minimally veneered just on the buccal side (Figure 11 through Figure 13).
For the conventional crowns, zirconia frameworks were fabricated from a white opaque zirconia (Prettau®, Zirkonzahn GmbH; other options include BruxZir [Glidewell] and KATANA [Kuraray Noritake]). After sintering (1600°C for 8 hours), the framework was tried on the cast and then veneered with feldspathic ceramic (IPS e.max® Ceram, Ivoclar Vivadent; other options include Creation [Jensen Dental] and Noritake Super Porcelain EX-3 [Kuraray Noritake]) in enamel and dentin shades, and glaze was applied and sintered (750°C for 1 hour).
The monolithic zirconia restorations were obtained from a high-translucent zirconia (Prettau Anterior®, Zirkonzahn GmbH; other options include Ceramill Zolid FX White [Amann Girrbach] and ArgenZ Anterior [Argen]). The crowns were pigmented and then sintered (1600°C for 8 hours); post-sintering pigmentation and finishing were also performed.
For the minimally veneered monolithic zirconia, complete crowns were digitally cut-back. After being machined, the crowns were pigmented and sintered (1600°C for 8 hours). The crowns were then minimally veneered with feldspathic ceramic just on the buccal side. After sintering, glaze was applied to improve the optical properties.
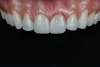
All crowns were tested and photographed under different lighting scenarios to evaluate their optical properties (Figure 5 through Figure 13). All photographs were taken with a DSLR camera with an EF 100mm f/2.8 Macro lens with different settings depending on the scenario. Crowns were clinically observed under natural light and also assessed in intraoral photographs with a dark background with the following camera settings: ISO 100, f/29, 1/125.
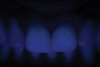
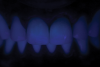
For fluorescence photographs, an ultraviolet light was used in a dark room with the following camera settings: ISO 3200, f/4, 1/100. For opalescence, a polarized filter was used and the camera settings were: ISO 800, f/5, 1/125.
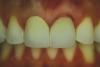
Finally, after evaluating all of the different crowns clinically and photographically, the patient and dental team selected the pair of crowns judged most similar to natural teeth. The conventional zirconia crowns presented a suitable high opacity from the zirconia framework and a fluorescence from the porcelain veneer that was higher than that of a natural tooth (Figure 5 through Figure 7). Conversely, the monolithic high-translucency crowns presented a lack of fluorescence, high opalescence, and a grayish aspect (Figure 8 through Figure 10). The pair of minimally veneered monolithic high-translucency zirconia (digital cut-back technique) crowns were selected for final cementation after presenting what were considered the best optical parameters that were most similar to natural teeth (Figure 11 through Figure 13). These crowns were thus cemented according to manufacturer instructions.
Follow-up was assessed at 3, 6, 12 (Figure 14), 24, and 32 months (Figure 15 and Figure 16). Optimal integration of restorations and soft tissues was evidenced at the follow-up visits. The patient was very satisfied with the esthetics and function.
Discussion
Minimally invasive dentistry aims to preserve and respect original tissues while simplifying clinical steps and achieving treatment goals in a predictable manner.17 Minimally invasive tooth extraction without flap releasing,3 followed by immediate implant placement and immediate provisionalization, are protocols associated with high success rates and are indicated to preserve the integrity of sound tissues when possible.1,4 This sequence of steps offers the possibility of producing final prostheses faster than a conventional two-stage implant protocol, because there is no need of a second surgery and the hard- and soft-tissue architecture can be maintained.18
After these objectives are achieved and osseointegration occurs, it is necessary to replace the interim restorations with definitive ones; however, cases that involve different substrates and colorations and the need to hide the varying colors represent a challenge for clinicians attempting to achieve natural-looking restorations.19 Conventional PFM crowns, commonly used for dental restorations, present several limitations due to the optical behavior of metal, which may be especially evident in the esthetic zone, as well as a black margin in cases where gingival recession or a thin biotype is present.20 To overcome these issues, all-ceramic restorations have been utilized, owing to the development of CAD/CAM systems, which offer digital workflows to obtain final restorations. Among the available materials to address this clinical situation, Y-TZP appears to be an interesting option because of its excellent flexural strength and fracture toughness as well as its optical properties.8 As a white, opaque ceramic, it is conducive to hiding unfavorably tinted substrates.14
The absence of translucency and fluorescence in first-generation zirconia, however, is considered a drawback in the pursuit of natural-appearing restorations; these characteristics are mandatory to veneering the framework with porcelain.10 Nonetheless, through this technique esthetic restorations may be obtained, however chipping of porcelain fired onto the zirconia framework has been noted as a critical problem.10 This is due mostly to the thermal coefficient mismatch and differences between the flexural strength of zirconia and the veneering porcelain, triggering cracking and other defects.21 Contrary to nature where fluorescence is higher in dentin,22 fluorescence in veneered zirconia restorations emanates from the outer layer of porcelain and not the framework. Increasing the feldspathic ceramic thickness could increase the degree of fluorescence but this may create an unnatural restoration.
Recently, the evolution of zirconia materials has enabled the use of third-generation monolithic high-translucency zirconia restorations with improved optical characteristics that offer a more natural appearance while eliminating the need for veneering, and thus avoiding porcelain chipping.11,23,24 However, the uniform translucency, low fluorescence, and high opalescence characteristics make this material unsuitable to hide unfavorable substrates and perform well in the esthetic zone.25 Another alternative is to use a digitally cut-back third-generation monolithic high-translucency zirconia restoration that is minimally veneered just on the buccal side. This approach reduces the amount of feldspathic ceramic on the surface, creating a synergy with the optical properties of the framework to more effectively mimic teeth fluorescence and translucency. This tactic, which also allows occlusal contacts to be on zirconia, offers both esthetics and appropriate performance while decreasing the possibility of porcelain chipping.26
Conclusion
The use of minimally veneered third-generation monolithic zirconia crowns may be an appropriate solution for obtaining esthetic restorations with optical properties that mimic those of natural teeth.
Acknowledgment
The authors thank the National Council for Scientific and Technological Development (CNPq), which supports Dr. Rafael. They also thank dental technician Marcelo Vieira, who made the restorations for this case.
About the Authors
Caroline F. Rafael, DDS, MSc, PhD
Postdoctoral Researcher, Department of Dentistry, Federal University of Santa Catarina,
Florianópolis, Brazil
Rodrigo M. Ferreira
MSc Student, Faculdade Inga (Uningá), Maringá, Brazil
Bernardo B. Passoni
Center for Education and Research on Dental Implants (CEPID),Federal University of Santa Catarina
Edwin Ruales-Carrera
PhD Student, Center for Education and Research on Dental Implants (CEPID),Federal University of
Santa Catarina
Cesar A. Benfatti
Professor, CEPID, Federal University of Santa Catarina
Anja Liebermann
Professor, Department of Prosthetic Dentistry, Ludwig-Maximilians Universität (LMU) München,
Munich, Germany
Claudia A. Volpato
Professor, Federal University of Santa Catarina
References
1. Jaju PP, Jaju SP. Clinical utility of dental cone-beam computed tomography current perspectives. Clinal, Cosmetic and Investigational Dentistry. 2014 Apr 2;6:29-43.
2. Pikos MA, Magyar CA, Llop DR. Guided full-arch immediate-function treatment modality for the edentulous and terminal dentition patient. Compend Contin Educ Dent. 2015;36(2):116,119-126,128.
3. Alzoubi F, Massoomi N, Nattestad A. Bone reduction to facilitate immediate implant placement and loading using CAD/CAM surgical guides for patients with terminal dentition. J Oral Implantol. 2016;42(5):406-410.
4. Emery RW, Merritt SA, Lank K, Gibbs JD. Accuracy of dynamic navigation for dental implant placement-model-based evaluation. J Oral Implantol. 2016;42(5):399-405.
5. Block MS, Emery RW, Cullum DR, Sheikh A. Implant placement is more accurate using dynamic navigation. J Oral Maxillofac Surg. 2017;75(7):1377-1386.
6. Balshi TJ, Wolfinger GJ, Balshi SF. Positioning handle and occlusal locks for the Teeth-in-a-Day protocol. J Prosthet Dent. 2016;115(3):274-277.
7. Parel SM, Triplett RG. Interactive imaging for implant planning, placement, and prosthesis construction. J Oral Maxillofac Surg. 2004;9:41-47.
8. Balshi SF, Wolfinger GJ, Balshi TJ. Surgical planning and prosthesis construction using computed tomography, CAD/CAM technology, and the internet for immediate loading of dental implants. J Esthet Restor Dent. 2006;18:312-325.
9. Balshi TJ, Wolfinger GJ, Alfano SG, et al. fabricating an accurate implant master cast: a technique report. J Prosthodont. 2015;24:654-660.