You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Using dental implants to assist and retain a removable prosthesis is a highly effective treatment and is an effective long-term option for edentulous patients.1-3While multiple approaches are utilized for implant overdenture design and construction, the most common application is the two-implant, tissue-supported, implant-retained removable prosthesis. Bar overdentures, however, also tend to be popular, especially when maxillary arches or patients with limited bone height are involved. Numerous factors related to successful treatment with overdentures include implant number, location, angulation, distribution, choice of abutment, and patient home care strategies.4,5
Many clinicians and technicians gravitate toward utilizing stud-style abutments-such as a LOCATOR (Zest Dental Solutions), Stern ERA (Sterngold Dental), and OT Equator (Rhein83)-due to simplicity related to clinical and technical processing methods and prosthetic space requirements. Stud-style abutment overdentures typically require 9 mm to 11 mm from the incisal edge of the prosthesis to the top of the implant platform, whereas bar overdentures typically require 13 mm to 15 mm from there.6-7 Consequences of insufficient prosthetic space include prosthesis fracture, excessive rotation of the prosthesis, insufficient retention, and bulkiness of the prosthesis. Many of these aforementioned clinical challenges are often not seen in the dental laboratory because technicians working on dental casts do not get responses from the patients indicating the bulkiness of the prosthesis of a bar overdenture prosthesis versus a stud-style overdenture prosthesis. As a result, clinicians tend to gravitate toward individual stud-style abutments to help address some of the clinical challenges associated with using a bar overdenture.
Much of what is accepted as standard technique regarding laboratory processing of overdentures is derived from our understanding of bar overdentures and traditional techniques related to tooth-/root-supported bar overdentures.8,9 The development of the science of utilizing titanium dental implants led to clinicians and technicians incorporating these classic root overdenture techniques into implant dentistry simply based upon analogous incorporation of the classic laboratory approach. Bar overdentures, as compared to stud-style abutment systems, typically are more implant-supported and have less resiliency compared to that of stud-style attachment systems. Resiliency of the attachment system is a mechanical property that is unique to removable prosthetics; it is defined as a mechanical force upon a tooth or dental implant that results from a combination of a spring-like function of mucosa deformation as a result of seating or biting forces of the prosthesis.10 An attachment that is considered resilient or semi-resilient is defined as one that permits a certain amount of movement of the prosthesis, typically within a rotation and/or vertical movement. Bar overdenture systems, such as the Hader Bar attachment system, are considered semi-resilient as they permit rotational movement but not vertical movement.11 Stud-style attachments are considered resilient or semi-resilient because they permit rotational and vertical movement of the prosthesis.
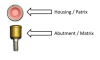
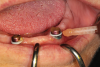
Implant overdenture attachment systems are typically made of several components: the abutment, the matrix, and the patrix. The abutment is the component that inserts directly into the dental implant and serves as a functional means of anchoring a prosthesis to the dental implant.10 The abutment typically serves as a matrix that permits attachment to the prosthesis using a retentive element, or patrix. The patrix is often comprised of a polymer, such as nylon or poly(ether) ether ketone (PEEK), which is under function and can withstand functional forces. The patrix insert is often encased by a metal housing that permits simple replacement when these forces result in wear of the polymer component (Figure 1).
Combining the patrix to the prosthesis is an important step in the clinical and laboratory procedures of fabricating the overdenture. Processing of the patrix portions of the overdenture attachment system typically involves using methacrylate-base resins, such as poly(methyl) methacrylate (PMMA), or bis-gma based resins, such as composite resins. Clinicians and technicians must choose whether to incorporate the housing/patrix indirectly in the dental laboratory using stone casts or directly intraorally with the patient assisting the procedure. The aim of this article is to discuss the benefits and limitations of each approach.
Laboratory Procedures
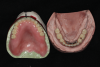
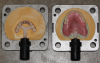
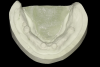
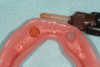
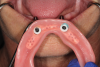
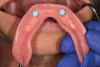
After a clinician has completed the impression procedure and tried in the prosthesis to confirm esthetics and tooth position, the laboratory completes the processing of the prosthesis. Prior to processing techniques, a technician creates a denture tooth assessment (also known as a wax-up), whereby denture teeth are suspended in pink baseplate wax onto mounted dental casts (Figure 2). The clinician has the patient return and places the proposed assessment onto the edentulous ridge to confirm the proper tooth, esthetic, and occlusal relationships, with the patient providing feedback. After confirming the aforementioned, the technician can begin processing procedures, which typically involve incorporating/flasking the denture tooth setup into a mold, followed by heating/boiling the mold until it reaches the melting point of the wax, when it is separated and the wax is washed away (Figure 3). This classic approach is often called a "lost-wax technique," as one is relying upon the low melting point of the wax to permit a simple separation procedure, leaving the denture teeth locked into one portion of the mold and the cast with the tissue surface or bar framework of the prosthesis in the other portion (Figure 4).
After the flasks have cooled, the technician prepares the dental mold to receive the acrylic resin to create the prosthesis. Acrylic resin processing procedures involve injecting/pouring/pressing of the resin into the mold created earlier; the resin polymerizes into the shape of the prosthesis created by incorporating the prosthesis into the mold during the lost-wax technique.8 The acrylic resin is heated using a controlled pressure environment to polymerize the resin and the technician removes the prosthesis to finish it by using polishing techniques.12
During the acrylic resin processing procedure, the technician has the choice to prepare a recess where the clinician can directly incorporate the housing during clinical procedures or the technician can incorporate the housing/patrix of the attachment system into the prosthesis during laboratory processing procedures. The former approach is facilitated by the clinician fabricating an impression of the edentulous arch containing the housing/patrix elements of the attachment system (Figure 5). During laboratory procedures, a positive stone cast version of the housing/patrix will act as a spacer for the prosthesis and will create the shape within the intaglio surface of the prosthesis. After processing, the technician enlarges the recesses slightly, creating an ideal recess for the clinician to process housings directly during chairside procedures with minimal adjusting needed within the prothesis. Incorporating retentive elements during laboratory procedures involves attaching the housings/patrices before, during, or after initial acrylic resin processing procedures. Attachment of the housing prior to or after acrylic resin processing procedures involves utilizing either the heat-processed acrylic resin during processing procedures or auto-polymerizing acrylic resin applied to the housing/patrix within the overdenture framework.
Laboratory Processing of Attachments
Polymerization of acrylic resin is an exothermic reaction, releasing both heat and energy. During this process, acrylic resin polymerization causes the material to shrink considerably, both in volumetric as well as linear dimensions.12 Heat-processed acrylic resin, used for bulk processing of denture bases, tends to shrink significantly more than auto-polymerization acrylic resin.13-14 Clinical and laboratory studies report that heat-processed acrylic resins show volumetric shrinkage ranges between 5% and 25%, whereas autopolymerizing acrylic resins show between 1% and 7% comparatively.8,13,14 Additionally, acrylic resin shrinks toward the center of mass of the void the resin is filling, so larger prostheses and those with uneven anatomical features tend to show greater distortion levels than others. Injection molding and controlling both heat and pressure in water-controlled environments tend to further help minimize distortion; however, distortion is still present.15
As a result, technicians are often concerned with using resin for processing of housing/patrices with tissue-supported overdentures or bar overdenture frameworks (Figure 6). Processing errors and distortion of between 1% and 25% may not be evident in tissue-supported complete dentures; however, they may be substantially more evident with overdenture attachment systems that are primarily tissue-supported and implant retained. Increasing the number of implants, adding a bar framework, and using non-resilient attachments systems tends to increase the amount of support derived from the implant attachment. Bar overdentures tend to be more implant-supported than stud-style attachment systems. Additionally, fabricating bar overdentures often involves having a stone cast with the bar on the cast, permitting the technician a tremendous amount of control to ensure processing techniques result in a prosthesis that is retentive and stable (Figure 7). As a result, a bar overdenture prosthesis may be an ideal prosthesis option for using laboratory processing of attachments compared to that of a tissue-supported complete denture.
When a clinician opts to perform a reline or rebase procedure of an implant-retained tissue-supported prosthesis, the amount of acrylic resin to be processed is substantially less than that of when the entire prosthesis is processed. As a result, a reline procedure permits simple workflows that allow the technician the ability to control the amount of acrylic resin shrinkage during processing procedures.16 Reline procedures permit the clinician to use the attachment system housing/patrix as a guide for the technician where he/she can utilize an impression made of the edentulous ridge within the prosthesis' intaglio surface and utilize them within the reline procedure (Figure 8). The technician can place a metal analog into the housing and, in combination with a laboratory reline jig, process a smaller amount of acrylic resin and directly incorporate the housings within the reline procedure itself (Figure 9). As a result, dimensional change is minimized and the prosthesis will have a greater chance of engaging the attachments evenly and precisely (Figure 10). Table 1 shows indications for laboratory processing of overdentures.
Chairside Processing of Attachments
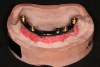
Stud-style attachment systems are engineered to maintain passivity over the implant system and tissue-bearing surface. The properties of these types of attachment systems often involve limited physical space, minimal framework, and short clinical height (Figure 11). The attachment system is intended to be utilized with limited implant support and the prostheses will be primarily tissue-supported and implant-retained.
When the technician and clinician use an indirect laboratory-clinical technique, the goal is to fabricate a prosthesis with recesses within the intaglio surface of the overdenture prosthesis prepared slightly larger than the housings/patrices to be attached. After laboratory procedures and prior to attaching the implant components, the clinician would adapt and adjust the prosthesis similar to that of any tissue-supported prosthesis prior to processing implant components (Figure 12). During this step, the clinician uses pressure-indicating media and selective adjustments to ensure the prosthesis is fully adapted to the edentulous ridge evenly prior to implant procedures. Due to the long-recognized understanding that some patients have easily displaceable soft tissues, which can result in substantial fit differences between the prosthesis on a stone cast versus intraorally, this singular step can substantially help to improve the fit of the prosthesis on the tissue-bearing surface.17 When fabricating a prosthesis for a patient with an edentulous ridge that is compressible and elastic and combining that with an attachment system that is resilient, it may be important to consider the above factors in combination with the understanding of volumetric shrinkage of acrylic resin. Additionally, a stud-style abutment with nylon or PEEK inserts has an on/off "fit" and when properly engaged, the patrix can properly retain and stabilize the denture. When the prosthesis is not properly engaged with the attachment system, however, the prosthesis may not have proper retention and stability.
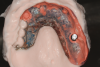
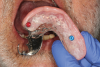
Chairside processing of housings/patrices are performed with the patient present and after the prosthesis has been fully adapted to the edentulous ridge without engaging the implants. A clinician can place a block-out spacer to prevent excess resin from flowing underneath the housings during processing of the attachments (Figure 13). The laboratory-prepared recesses are slightly enlarged using acrylic burs specific to stud-style attachment systems and mechanical undercuts are placed within the prosthesis (Figure 14). Additionally, a hole is prepared between the recess and the cameo, or outside, surface of the prosthesis to act as a vent so any excess resin can flow out the prosthesis and not onto the edentulous ridge. Acrylic or composite resin is flowed into the prepared recess and the clinician seats the prosthesis onto the edentulous ridge (Figure 15 and Figure 16). Some clinicians prefer to have the patient close into centric or bite down during this step; however, many believe that this can increase displacement of the soft tissues. As a result, some prefer to hold the prosthesis on the edentulous ridge, evenly applying pressure to ensure excessive biting pressures are prevented. This approach can potentially result is an evenly adapted tissue-supported, implant-retained prosthesis compared to the potential of having a prosthesis not evenly seated onto the edentulous ridge due to the patient not evenly closing into centric. This approach, furthermore, can maximize tissue support and minimize implant support of the final prosthesis. After the resin has completely polymerized, the prosthesis is removed and inspected to ensure housings/patrices are properly attached and minimal resin displaced onto the edentulous ridge (Figure 17). Processing inserts are changed for retentive inserts, the prosthesis is placed onto the edentulous ridge, and implants are engaged to confirm complete adaptation and proper retention and stability of the prosthesis (Figure 18).
When evaluating a tissue-supported, implant-retained prosthesis with a resilient stud-style attachment system, it is important to consider the passivity of the prosthesis when fully engaged in the implant system. Using chairside processing steps can potentially increase the ability of the clinician to fabricate a prosthesis that properly engages the implants.18 Additionally, some have shown in clinical studies that chairside attachment processing results in fewer pressure sore spots, fewer visits to the clinician for retentive element adjustments, and minimizing long-term mechanical problems with the prosthesis.19
Closing Comments
Clinical and laboratory procedures to fabricate implant overdentures involve a close collaboration between clinician and technician to ensure an optimal outcome. Multiple laboratory steps are involved that can potentially result in dimensional changes within the prosthesis and how it can affect the final retention and stability of the prosthesis. Laboratory processing of housings/patrices is recommended when fabricating a bar overdenture or when the amount of processed acrylic resin is minimal, such as with a reline. Chairside processing of housings/patrices can enhance the retention and stability of overdentures that use stud-style resilient attachment systems.
About the Author
Michael D Scherer, DMD, MS
Private Practice
Sonora, CA
Assistant Clinical Professor
School of Dentistry, Loma Linda University
Loma Linda, CA
References
1. Naert I, Alsaadi G, Quirynen M. Prosthetic aspects and patient satisfaction with two implant-retained mandibular overdentures: a 10-year randomized clinical study. Int J Prosthodont. 2004;17:401-10.
2. Sadowsky SJ. Mandibular implant-retained overdentures: a literature review. J Prosthet Dent. 2001;86:468-73.
3. Scherer MD. Overdenture Implants. A Simplified and Contemporary Approach to Planning and Placement. Dent Today. 2015;34:54, 56-8, 60.
4. Scherer MD, McGlumphy EA, Seghi RR, Campagni WV. Comparison of retention and stability of implant-retained overdentures based upon implant number and distribution. Int J Oral Maxillofac Implants. 2013 Nov-Dec;28(6):1619-28.
5. Scherer MD, McGlumphy EA, Seghi RR, Campagni WV. Comparison of retention and stability of 2 implant-retained overdentures based upon implant location. J Prosthet Dent. 2014 Sep;112(3):515-21.
6. Phillips K, Wong KM. Space requirements for implant-retained bar-and-clip overdentures. Compend Contin Educ Dent. 2001;22(6):516-518, 520, 522.
7. Lee CK, Agar JR. Surgical and prosthetic planning for a two-implant-retained mandibular overdenture: a clinical report. J Prosthet Dent. 2006;95(2):102-105.
8. Brewer AA, Morrow RM. Overdentures. 2nd ed. St. Louis, MO: Mosby; 1985. p. 208-51
9. Choy E, Reimer D. Laboratory processing of housing-retained attachments for implant-supported overdentures. J Prosthet Dent. 2001;85(5):516-518.
10. The glossary of prosthodontic terms: ninth edition. J Prosthet Dent. 2017;117(5S):e1-e105.
11. Barão VAR, Assunção WG, Tabata LF, de Sousa EAC, Rocha EP. Effect of different mucosa thickness and resiliency on stress distribution of implant-retained overdentures-2D FEA. Comput Methods Programs Biomed. 2008;92(2):213-223.
12. Anusavice K, Shen C, Rawls HR. Phillips' Science of Dental Materials. Saunders; 2012.
13. Firtell DN, Green AJ, Elahi JM. Posterior peripheral seal distortion related to processing temperature. J Prosthet Dent. 1981;45(6):598-601.
14. Mojon P, Oberholzer JP, Meyer JM, Belser UC. Polymerization shrinkage of index and pattern acrylic resins. J Prosthet Dent. 1990;64(6):684-688.
15. McLaughlin JB, Ramos V, Dickinson DP. Comparison of fit of dentures fabricated by traditional techniques versus cad/cam technology. J Prosthodont. 2019;28(4):428-435.
16. Barco MT, Moore BK, Swartz ML, Boone ME, Dykema RW, Phillips RW. The effect of relining on the accuracy and stability of maxillary complete dentures--an in vitro and in vivo study. J Prosthet Dent. 1979;42(1):17-22.
17. Hanau RL. The relation between mechanical and anatomical articulation. JADA. 10: 776-784, 1923
18. Bidra AS, Agar JR, Taylor TD, Lee C, Ortegon S. Techniques for incorporation of attachments in implant-retained overdentures with unsplinted abutments. J Prosthet Dent. 2012;107(5):288-299.
19. Nissan J, Oz-Ari B, Gross O, Ghelfan O, Chaushu G. Long-term prosthetic aftercare of direct vs. indirect attachment incorporation techniques to mandibular implant-supported overdenture. Clin Oral Implants Res. 2011;22(6):627-630.