You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
A worn dentition is one of the more challenging scenarios a practitioner can face. An aging population and esthetically driven patient demands have created an increased need for restorative teams to be able to offer different treatment modalities for this condition. Epidemiological studies show that the proportion of adults with severe tooth wear generally rises from approximately 3% among young people in their early 20s to 17% among those aged 70 and older.1 Understanding how wear occurs and what restorative materials should be used can inform the laboratory professional in finding ways to address such cases.
Classifications of Tooth Wear
It is important to note that "wear" is not a diagnosis; it is merely an objective indication of a medical fact. A diagnosis is the determination of the cause of the wear, which can be of functional, chemical, or abrasive origin.2 These distinct classifications reinforce the belief that these processes occur individually; however, in clinical reality, it is much more likely that the practitioner will face a combination of etiologies.3
Attrition
Attrition is defined as tooth wear that results from tooth-to-tooth contact. Physiological (ie, normal) tooth wear occurs at a rate of about 20 to 40 µm per year. Pathological (ie, abnormal) tooth wear is the result of bite problems, such as a frictional chewing envelope with too much contact of the front teeth during functional chewing movements, which typically results in accelerated wear of the front teeth; a dysfunctional chewing envelope with enlarged chewing strokes due to uneven posterior contacts, which typically results in anterior and posterior wear4; or the result of parafunction, which is brain mediated, can be caused by certain medications, and is often related to sleep-disordered breathing.5Abnormal attrition will typically result in posterior and lateral wear. A correct diagnosis of abnormal tooth wear requires a detailed dental and medical history, a clinical examination, and a functional analysis.
Abfraction
Abfraction is the result of biomechanical loading forces. Tooth flexure arising from cyclic, eccentric occlusal forces results in the formation and progression of defects in vulnerable cervical regions of the teeth. Abfraction expresses as wedge-shaped defects at the cemento-enamel junction of the teeth. The etiology, however, is controversial, because the lesion progression is most likely accelerated by abrasive components. In addition to a detailed medical and dental history, correct diagnosis will require a clinical examination with a focus on areas of possible occlusal overload.6
Erosion
Erosion is defined as the loss of dental hard tissues from non-bacteriogenic acid, which can be either dietary or gastric. Evidence suggests that erosion may be becoming more prevalent due to the increased popularity of carbonated beverages, particularly among the younger generation, and gastric acid-related issues, namely gastroesophageal reflux disease (GERD) and bulimia. These conditions cause more severe expressions of tissue loss due the much lower pH of gastric acid when compared with dietary acids. Depending on the etiology, the hard tissue loss from erosion presents at different sites. Dietary acid-related erosion will mostly affect the buccal and occlusal tooth surfaces, particularly when combined with a swishing habit or overzealous brushing. Gastric acid erosion tends to present more on the palatal surfaces of the upper anterior segment, particularly in cases involving bulimia, in which the tongue will rub against the upper front teeth during vomiting (ie, perimylolysis).7Erosion from GERD will often present more severely on one side of the mouth, correlating with the patient's sleeping posture. All gastric acid-related issues can also affect the occlusal surfaces of the posterior teeth. Erosion and attrition often occur concomitantly, and a clinical presentation of dentinal cupping will typically exist when erosion is outpacing attrition. In addition to a medical and dental history and a clinical examination, diagnosis will include a dietary analysis. It has to be stressed that a gentle questioning approach is required in cases where bulimia is suspected.
Abrasion
Abrasion describes the pathological and mechanical wearing of dental hard tissues by foreign objects that are repeatedly introduced into the mouth. Depending on the etiology, it may present as localized (eg, caused by toothpicks) or diffuse. The most common clinical presentation is brushing abrasion, which can be caused by overbrushing and abrasive dentifrices. A dental and medical history, as well as the intraoral presentation on examination, will aid in a correct diagnosis of dental abrasion.8
Treatment Considerations
The successful management and treatment of tooth wear, which depends on a correct diagnosis, the amount of hard-tissue loss, symptoms (eg, sensitivity, pain), and the age of the dentition (ie, deciduous, permanent), can range from lifestyle modifications (eg, dietary acid intake, brushing technique, choice of dentifrice), medications, and counseling (eg, in cases involving gastric acid) to simple restorative treatment (eg, non-carious cervical lesions) and very complex restorative treatment plans in cases with more advanced attrition.3
When wear is more advanced, particularly in the anterior segment, patients often want to simply restore their teeth to their appropriate appearance and can be baffled when told that to accomplish this, more complicated dentistry, possibly including orthodontics or the treatment of at least one full arch, may be required. A number of approaches can be used, including laboratory-fabricated indirect restorations, which can yield longer-term results in many cases. In this particular case, the team chose direct composite restorations to address the issue. In order to phase treatment and provide patients with a lower cost entry point, transitional composite bonding can be utilized. This article describes the successful treatment of such a case using a mixture of direct and indirect composite bonding techniques.
Case Report
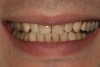
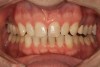
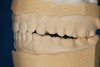
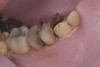
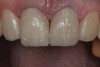
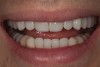
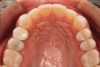
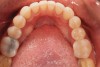
A 34-year-old male patient with no medical issues presented to the office with the chief complaint of a failing crown on tooth No. 12. The patient was also unhappy with his bite and the appearance of his teeth (Figure 1 and Figure 2).
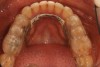
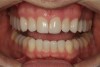
Over time, the patient had developed joint and muscle symptoms due to his lack of posterior support and sought the help of a specialist. His bite was analyzed, and he was fitted with a dental orthotic that allowed his teeth to touch in centric relation (Figure 3). This was intended to be a temporary measure to stabilize the patient's bite and make him comfortable, but before any permanent treatment could be carried out, he moved abroad and had been living with the device for more than 4 years before the time of the consultation. He stated that his bite was now very stable with the orthotic, but he was looking for a more permanent solution and also wanted to improve the overall appearance of his smile.
Clinical Examination and Findings
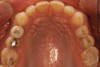
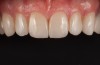
A comprehensive examination was carried out, and preoperative photographs were taken (Figure 1 through Figure 4). The patient presented with fair oral hygiene and slight, generalized tissue inflammation. Caries and defective restorations were detected on teeth Nos. 4, 5, 13, and 14. The crown on tooth No. 12 was showing signs of leakage, and although the endodontic access cavity had been temporarily restored with composite, this endodontic re-treatment was acceptable and the tooth was otherwise symptom-free. Erosion was present on most of the posterior teeth and the cuspids, and abrasion was noted on teeth Nos. 4, 5, 10, 11, 20, 21, 22, 28, and 29. An examination of the patient's muscles, joints, and bite revealed no joint sounds, a normal range of motion, and negative joint load and immobilization tests.
The patient's removable dental orthotic covered the lower bicuspids and first molars. With the orthotic in place, there was shim stock contact on all posterior teeth and on the second molars that were not covered by the appliance. However, there was no incisal overlap and a lack of anterior guidance.9When the orthotic was removed, no more than three teeth touched, and a 2-mm space between the posterior teeth made mastication difficult.
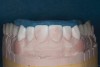
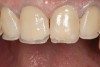
The dentofacial examination revealed a low smile line with no incisor display when the lips were in repose. The anterior teeth were chipped and worn, and their overall color was darkened. The buccal corridors were deficient, and the failing crown on tooth No. 12 was visible in a full smile.
Treatment Plan
Periodontal therapy consisting of scaling and polishing would be provided, with a focus on increasing home care and maintaining 6-month recall intervals. Treatment of the decay, coverage of all of the eroded and abraded surfaces, and a new crown on tooth No. 12 would also be required. It is important to note that once dentine is exposed, it will wear at a rate of at least three times the average wear rate of enamel, even in the absence of causative erosive factors.10,11
Confirmed by the mounted models (Figure 5), the patient's bite was obviously unsatisfactory, but with the orthotic in place, he was completely symptom-free and stable, and therefore, considered to be in acceptable function. However, he was considered to be in occlusal dysfunction without it because he lacked simultaneous, equal-intensity posterior contacts.
Based on multiple factors, the decision was made to close the posterior open bite and create anterior guidance using additive means in the patient's current maximum intercuspation, which was considered equivalent to centric relation. He would then be equilibrated to ensure even, simultaneous posterior contacts and canine guidance.
Restorative material options, namely porcelain and composite, were discussed with the patient. Because he preferred to have no tooth structure at all removed during this stage, and porcelain onlays would have necessitated some preparation of the posteriors because of the minimal thickness requirements,12the decision was made to restore him with additive composite onlays for his posterior teeth to establish occlusion and composite veneers for his upper anterior teeth and bicuspids to address his esthetic needs and cover the existing buccal abrasions. Only tooth No. 12 would receive a porcelain restoration.
The reduced cost of these material choices was an important factor in the patient's decision-making process. To further minimize cost, the posterior units would be produced using a time-saving wax-up duplication technique by a dental technician. It was explained to the patient that the life expectancy of the posterior composite onlays was limited, and that he would eventually have to switch to a more durable option, such as porcelain.
In addition, the lower anterior teeth would be bleached, and the abrasions on the lower bicuspids would be covered with composite restorations.
Treatment
Accurate vinyl polysiloxane impressions (Take 1, Kerr Corporation; kerrdental.com) were taken of the upper and lower arches. Two sets of models were obtained and mounted in a Panadent articulator (Panadent Corporation; panadent.com). A diagnostic wax-up to close the posterior open bite and incorporate the desired esthetic changes was carried out on one of these sets. The posterior waxed-up surfaces were then duplicated with a clear silicon matrix (RSVP, Cosmedent; cosmedent.com) in quadrants. These matrices were loaded with a slightly warmed microhybrid composite (Four Seasons, Ivoclar Vivadent; ivoclarvivadent.com) and seated onto the corresponding second model, which had been isolated with a separating agent. Warming the composites increases monomer conversion, thereby decreasing curing time and shrinkage.13 Once fully cured, the occlusion was adjusted, and the onlays could easily be separated from the models. (The author acknowledges that with today's technology, she would probably opt for a millable composite; a laboratory-produced, long-term provisional material; or a direct-injectible, high-strength composite and a matrix technique.)
Following caries treatment and tooth preparation (Figure 6), teeth Nos. 4 through 13 were restored with direct composite veneers in stages (Figure 7 through Figure 9). Using a hybrid composite for the lingual shelf and dentin layer provides wear resistance and strength for the restoration.14,15 (The lowest wear rates for restorations and the opposing dentition occur with metal alloys, machined ceramics, and microfilled hybrid resin composites. Any adjusted and unpolished porcelain surface would elicit the most wear on the opposing teeth.11)After the composite veneers were finalized, a monolithic lithium disilicate crown was placed on tooth No. 12 during a subsequent appointment, and occlusal equilibration was carried out. Final photographs were taken a couple of weeks later (Figure 10 through Figure 14).
Conclusion
The use of transitional bonding techniques can allow complex cases to be treated in a cost-effective and timely manner. Furthermore, occlusal and esthetic designs can be evaluated while the maximum amount of tooth structure is conserved.
About the Author
Sandra Hulac, DDS
Private Practice
Hong Kong, China
References
1.Van't Spijker A, Rodriguez JM, Kreulen CM, et al. Prevalence of tooth wear in adults. Int J Prosthodont. 2009;22(1):35-42.
2. Hattab FN, Yassin OM. Etiology and diagnosis of tooth wear: a literature review and presentation of selected cases. Int J Prosthodont. 2000;13(2):101-7.
3. Hannif A, Rashid H, Nasim M. Tooth surface loss revisited: Classification, etiology, and management. J Res Dent. 2015;3(2):37-43.
4. Kois JC. New challenges in treatment planning: incorporating the fundamentals of patient risk assessment - Part 2. J Cosmet Dent. 2011;27(1):110-121.
5. Rouse JS. The Bruxism Triad: Sleep bruxism, sleep disturbance, and sleep-related GERD. Inside Dentistry. 2010;6(5):32-44.
6. Antonelli JR, Hottel TL, Garcia-Godoy F. Abfraction lesions--where do they come from? A review of the literature. J Tenn Dent Assoc. 2013;93(1):14-9; quiz 20-1.
7. Winter R. Bulimia: Complex Etiology, Challenging Treatment. Dent Today. 2015;34(7):119-20, 122-3.
8. Grippo JO, Simring M, Coleman TA. Abfraction, abrasion, biocorrosion, and the enigma of noncarious cervical lesions: a 20-year perspective. J Esthet Restor Dent. 2012;24(1):10-23.
9. Ash MM. Current concepts in the aetiology, diagnosis and treatment of TMJ and
muscle dysfunction. J Oral Rehabil. 1986;13(1):1-20.
10. Larson TD. Tooth wear: when to treat, why, and how. Part two. Northwest Dent. 2009;88(6):19-28.
11.Yip KH, Smales RJ, Kaidonis JA. Differential wear of teeth and restorative materials: clinical implications. Int J Prosthodont. 2004;17(3):350-6.
12. IPS e.max All Ceramic Chairside Preparation Guide. IPS e.max Lithium Disilicate Martial Science, Practical Applications. Published by Ivoclar Vivadent.
13. Freedman G. Clinical benefits of pre-warmed composites. Private Dent. 2003;8(5):111-14.
14. Hervás-García A, Martinez-Lozano MA, Cabanes-Villa J, et al. Composite Resins. A review of the materials and clinical implications. Med Oral Patol Oral Cir Bucal. 2006;11(2):E215-20
15. Lambrechts P, Vanherle G. Structural evidences of the microfilled composites. J Biomed Mater Res. 1983;17(2):249-60