You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Knowledge regarding temporization of implant dentistry and techniques relating to the process of fabricating implant-supported provisional prostheses are important for any member of the dental team. When a patient requires implant-supported prosthetics, the dentist has two choices: fabricate a provisional implant-supported prosthesis prior to the fabrication of the definitive prosthesis, or directly fabricate the definitive prosthesis without a provisional. Placement of a provisional prosthesis can enhance the final esthetic outcomes of the treatment.1 Wittneben, et al, defined optimal esthetic implant restoration as "a combination of a visually pleasing prosthesis and surrounding peri-implant soft tissue architecture."2Achieving esthetically superior outcomes depends not only on prosthetic management but also on surgical placement and the presence of adequate bone and soft tissue support.
Advantages of Temporization
Temporization of implant-supported prostheses offers several advantages. It provides patients with function and esthetics during treatment time.3 It enhances esthetics by contouring soft tissue architecture and emergence profile prior to fabrication of the definitive prosthesis-an especially important consideration in the anterior segments.2 It provides ideal tools for proper communication with the dental laboratory technicians during fabrication of the definitive prosthesis, with the emergence profile previously tested and accepted by the patient.3,4
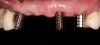
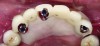
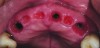
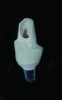
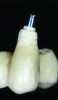
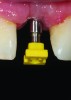
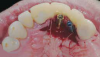
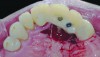
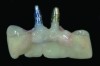
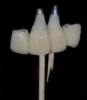
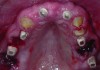
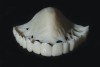
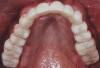
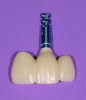
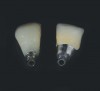
Temporization also helps with the analysis of form, function, and patient expectations.4 It simplifies prosthetic procedures such as occlusal registration and delivery of the definitive prosthesis. Additionally, it helps to form and maintain the shape of a pontic receptor site in cases where that is present as part of the implant-supported prosthesis (Figure 1 through Figure 4). Finally, it reduces the chances of tipping of adjacent teeth or extrusion of the opposing segment, minimizing adjustments during the delivery appointment for the definitive prosthesis.5
Obtaining the ideal emergence profile is necessary not only for providing a definitive implant-supported prosthesis with ideal esthetics but also for aiding the laboratory in fabricating a cleansable definitive prosthesis. Frequently, when a dentist makes a definitive impression after removal of the healing abutment-which usually has a narrower diameter at the gingival margin than is desired for the prosthesis-without prior fabrication of a provisional restoration, the laboratory will have two choices: Either duplicate the same emergence or grind from the soft tissue model in the working cast before fabricating the prosthesis, which will allow fabrication of a definitive prosthesis with better emergence profile.6
The primary disadvantage of grinding from the soft tissue model is the subsequent need for extended chairside time during appointments for try-in and delivery of the definitive prosthesis. Furthermore, the esthetics of the definitive prosthesis may be compromised after healing.
If the laboratory does not alter the soft tissue model and chooses to fabricate a prosthesis using the same emergence profile provided by the dentist. The resulting restoration will most likely have an abrupt emergence profile that may contribute to plaque accumulation and difficulty in performing proper oral hygiene measures by the patient.
In order to overcome this obstacle, a provisional prosthesis or a customized healing abutment should be fabricated prior to making the definitive impression. The custom healing abutment may be made conventionally, using a screw-retained abutment and flowable composite resin7 or digitally milling a customized healing abutment.8,9
Temporization Time
Temporization can be accomplished immediately after implant placement. (Immediate loading is defined as being within 72 hours of implant placement.10,11) Temporization is also possible during any other phase of the treatment, such as a Stage II implant uncovering procedure or after placement of the healing abutment and healing of the soft tissue.
The benefits of immediate loading include:
•
Providing patients with immediate replacement of missing teeth and esthetics.
•
Allowing the dentist to place a fixed restoration instead of a removable prosthesis.
•
Allowing for less bone and soft tissue loss after surgery. In a study by Tarnow, et al, immediate flapless implant placement in addition to placement of a bone graft material in the facial gap-which is located between the implant and facial bone-in combination with a fixed provisional prosthesis or custom healing abutment resulted in the smallest ridge contour changes.12
•
Helping to maintain or sculpt the soft tissue and emergence profile immediately after implant placement.5
•
Helping with maintenance of inter-arch space.5
•
Providing higher comfort and function for the patients.3,5
•
Eliminating the need for second-stage surgery.5
•
Allowing provisional prostheses with proper contours to act as surgical guides.13,14
The requirements for immediate loading include little or no bone loss being present around the implant, and adequate primary stability; it is recommended to have 3 mm to 5 mm of bone beyond the apex and bone length of 10 mm or more for stability.15-18
There are several contraindications to immediate loading.18 When an implant is unable to endure an applied torque of 35 Ncm to 40 Ncm without its rotation, it is considered to lack the primary stability, and there is a relative contraindication to load that implant immediately when there is a lack of primary stability,19,20 though "this deficiency may be overcome with multiple-unit splinting," according to Bahat.18 Other contraindications include a lack of posterior occlusal support, the presence of periodontally mobile teeth, and parafunctional habits or powerful facial musculature.
Components
A provisional implant prosthesis consists of a temporary abutment and provisional material. It can be either cement- or screw-retained.
Cement-retained provisional prostheses are easier to fabricate but introduce a risk of excess residual cement, especially if the abutment margin is subgingival. Screw-retained provisional prostheses provide better ability to shape the tissue and provide ideal emergence profile for the definitive prosthesis.3
Several options exist for abutment material. Titanium (Figure 2) is used mainly for screw-retained provisional prostheses. Titanium abutments are stronger than PEEK abutments and may provide for longer-term provisionals. PEEK (Figure 5) is used mainly for cement-retained prostheses. It does not bond to acrylic and usually offers different heights for finish line locations and different emergence profiles. Preparation to reduce emergence profile and move the location of the finish line apically can be easily accomplished, but additions are difficult due to the fact that acrylic does not bond well to it. Screw-retained PEEK abutments are also available with mechanical undercuts; surface conditioning of the abutment can be made to enhance mechanical interlocking and adhesion for screw-retained provisional restorations. A screw-retained PEEK abutment also can be converted to a cement-retained provisional abutment via the addition of flowable composite to the subgingival portion of the abutment in order to obtain the desired emergence profile, as well as preparation and smoothening of the axial surfaces21 (Figure 5 and Figure 6).
Other materials, such as PMMA, can be screw- or cement-retained.
The connecting interface of the abutment with the implant can be either engaging or non-engaging with the implant. A non-engaging abutment can rotate 360°, while an engaging abutment does not allow any rotation. Engaging abutments are used for all single-unit restorations (cement- and screw-retained). In Figure 14, the left is non-engaging and the right is engaging; notice the engaging hex. Cement-retained provisional abutments should always be engaging as well. Non-engaging abutments are used for screw-retained implant-supported fixed partial dentures (multiple splinted units) for ease of seating and more passive fit.22 Some practitioners choose one engaging and the rest non-engaging abutments when fabricating splinted multiple units for implant-supported fixed partial dentures.
Worth noting is that a definitive abutment can be fabricated to which an implant-supported provisional prosthesis is attached.
To give the desired shape for the provisional prosthesis, the following should be used: vacu-form matrix,23 preformed crown,24 laboratory-processed provisional shells,25 denture teeth, putty matrix, and extracted teeth.26, 27 A removable complete denture can also be converted to a fixed provisional prosthesis in full-arch cases,28,29 which is beyond the scope of this article.
Core materials include PMMA,24 Bis GMA (Bis-phenol A glycidyl methacrylate),23 light-cured composite resin,23 and others.
Temporization Techniques
The process of fabricating an implant-supported provisional prosthesis may be undertaken in one of three manners: chairside by the dentist; laboratory-processed by the dental technician; or a combination of both the dental technician and the dentist, depending on the circumstances and method preferred by the dentist.3,21,23-25,30
Laboratory-Processed Provisional
The clinical steps for a laboratory-fabricated provisional prosthesis include obtaining a fixture-level impression using open- or closed-tray impression techniques (Figure 7); obtaining an occlusal registration; obtaining an opposing impression; obtaining a facebow record if needed; and obtaining photos and a shade.6
After the dental technician waxes up (or digitally designs) and fabricates the provisional prosthesis (Figure 8 and Figure 9), it should be tried in and adjusted. (The try-in process for provisional prostheses is similar to that of definitive prostheses). Adjustments may be made to achieve better contact areas, supragingival contours, and subgingival contours, as well as to obtain the ideal emergence profile and proper occlusion.
Screw-Retained Provisionals
With chairside fabrication of the provisional prosthesis, screw retention is generally preferable to cement retention due to the ease of altering emergence profile, higher retention, and lack of cement interface.31
Several techniques, using any of the previously mentioned prosthesis formers, have been mentioned in literature.3,21-25,30,32 The technique that will be discussed here involves the use of laboratory-processed provisional shells made from PMMA. The core materials that are used to connect, fill, and create emergence profile are a combination of PMMA and flowable light-cured composite resin.
The provisional shells should have a positive stop or support that guides them to seat accurately.33 Otherwise, a separate jig made of transparent vacu-form stent material can be used to orient the shells in the patient's mouth in the same exact manner as the cast on which they were fabricated. The positive stops or acrylic support may be placed on adjacent prepared teeth as in the current technique, on the palate, or on the ridge33 (Figure 3).
The technique frequently chosen by the author includes the use of a stop made from the same PMMA material as the shell due to its simplicity:
1.
The provisional abutments are tried in after removal of the cover screw or healing abutment from the implant.
2.
After being marked with a marker intraorally, the height of the provisional abutment is then adjusted extraorally until it does not interfere with the occlusion (high-speed handpieces and carbide burs can be used for titanium abutments).
3.
A window is opened palatally/lingually on the shell using low-speed and carbide acrylic burs, and the provisional shells are seated, verifying complete seating of the provisional prosthesis. Adjust the provisional abutment and/or the provisional shells further if necessary until the provisional restorations seat passively (Figure 10).
4.
Close access holes of the abutments using PTFE (polytetrafluoroethylene) tape or cotton and a temporary restoration material. PVS (polyvinyl siloxane) material can also be used to seal and fill access holes.
5.
A piece of rubber dam material can be used to protect the surgical site if needed.
6.
Use PMMA or flowable composite to attach the provisional shells to the provisional abutments (Figure 11). Before attaching, check position, esthetics, phonetics, and occlusion.
7.
After adding an adequate amount and complete setting of the core material, remove from the mouth (Figure 12).
8.
Add more PMMA or flowable composite to deficient areas and emergence areas (Figure 13).
9.
Shape to give proper contours subgingivally and supragingivally. Implant-supported units can be separated from the teeth-supported units if present (Figure 13).
10.
Place on an implant laboratory analog and polish adequately (Figure 14).
11.
Place in the mouth, tighten, recheck occlusion, and adjust if necessary. Repolish and seal the access holes of the provisional prosthesis with appropriate material.
Cement-Retained Provisionals
Cement-retained provisional prostheses may be useful in some instances, and they are generally easier to fabricate. In case of limited inter-arch space, a screw-retained abutment is preferable in the provisional phase as well as in the definitive phase.31
The dentist first must choose the appropriate PEEK provisional abutment that has adequate gingival collar height and width, depending on the soft tissue thickness, location of the implant platform, and location in the mouth. The emergence profile of the prosthesis will be created by the gingival collar portion of the provisional abutment (the dentist should always use a height and width greater than expected because removal later is much easier than addition).
The provisional abutment is then tried in and the gingival collar height adjusted to give proper equigingival or slightly supragingival finish lines. Adjustments should be done extraorally after being marked intraorally using a marker (high-speed crown preparation burs can be used).
The height should be adjusted to give 2 mm of occlusal clearance (Figure 15). The dentist can then adjust facial, lingual, and proximal contours in a manner similar to axial preparation of the teeth for the full-coverage crown restorations (Figure 15); note that the implants in this case were not loaded immediately; some were loaded during the uncovering procedure and extraction of the posterior teeth. Remaining teeth will be extracted at a later appointment. Immediately loaded implants should not be splinted to teeth.
The dentist then tries in the laboratory-processed provisional shells and makes sure the shells are fully seated (Figure 16). Further adjustments can be made to the shells and/or temporary abutments until they fully seat. The palate was utilized in this case for the positive stop or acrylic resin support33 to ensure complete seating of the provisional shells, as mentioned earlier. Occlusion should also be checked.
The access holes of the provisional abutment are then sealed with cotton or PTFE tape and an interim restoration material; PVS material can also be used. The dentist relines the laboratory-processed shells with a material of choice. (PMMA will allow easier bonding to the provisional shells.) Before relining, the position, esthetics, phonetics, and occlusion should be verified.
After setting, the dentist can remove the shell, contour, and trim the excess material around the margins in a manner similar to conventional teeth-supported provisional techniques. The positive stop portion that was used also should be trimmed (the palatal stop, in this case).
The abutment is then placed on an implant laboratory analog and polished adequately, and the provisional prosthesis should be polished as well. The provisional prosthesis is tried in, and the dentist rechecks occlusion and cement using temporary cement material, and cleans excess cement (Figure 17).
Transferring Emergence Profile
After creating ideal esthetics and emergence profile, the dentist should provide the laboratory technician the information necessary to fabricate a definitive prosthesis. A final impression with an emergence profile identical to that of the provisional restoration should be obtained. If the provisional is removed, the tissue will collapse and the emergence might change in the final impression. Different techniques for transferring the exact emergence have been discussed in the literature, including the use of the custom impression coping.3,4,34
The implant-supported provisional prosthesis is connected to a laboratory analog (Figure 18). Stone is poured in a medicinal cup, and the connected provisional is placed. The stone should be at a lower level than the coronal aspect of the analog (it is useful to have analogs in a medicinal cup for later use). Low-viscosity PVS material is poured in the medicinal cup on top of the set stone; the entire subgingival emergence profile portion of the provisional prosthesis must be captured (Figure 19). After the PVS material is set, the provisional prosthesis is removed (Figure 20). An impression coping is screwed to the analog, and chemically cured or light-cured resin is flowed in the gap between the abutment and the PVS material to capture the emergence profile created by the provisional prosthesis (Figure 21). The resin can also be added to an adjacent pontic site to capture ovate pontics if present.35 Once the resin is set, the impression coping is unscrewed from the analog and placed in the patient's mouth with the same orientation as the provisional; it is helpful to mark the buccal surface of the resin on the impression coping (Figure 22). A radiograph may be taken to ensure complete seating of the impression coping on the implant inside the patient's mouth. The impression is then made; it will contain an exact replica of the emergence profile of the provisional prosthesis.
The dental technician can duplicate the same emergence obtained with the provisional for the final prosthesis (Figure 23).
Conclusion
Frequently, clinical outcomes of implant-supported prostheses are compromised due to the dentist's inability to provide the proper prosthetic management and necessary information to the dental laboratory technician. A provisional restoration not only provides patients with enhanced comfort during treatment time but also aids the dental technician in the fabrication of a predictable, cleansable definitive prosthesis.
About the Author
Ali Nazar, BDS
Prosthodontist
Clinical Research
Master's Candidate
New York University College
of Dentistry
New York, NY
References
1. Furze D, Byrne A, Alam S, Wittneben J-G. Esthetic Outcome of Implant Supported Crowns With and Without Peri-Implant Conditioning Using Provisional Fixed Prosthesis: A Randomized Controlled Clinical Trial. Clinical Implant Dentistry and Related Research. 2016;18(6):1153-1162. doi:10.1111/cid.12416.
2. Wittneben J-G, Buser D, Belser UC, Brägger U. Peri-implant Soft Tissue Conditioning with Provisional Restorations in the Esthetic Zone: The Dynamic Compression Technique. The International Journal of Periodontics and Restorative Dentistry. 2013;33(4):447-455. doi:10.11607/prd.1268.
3. Santosa R. Provisional restoration options in implant dentistry. Australian Dental Journal. 2007;52(3):234-242. doi:10.1111/j.1834-7819.2007.tb00494.x..
4. Papadopoulos I, Pozidi G, Goussias H, and Kourtis S. (2013). Transferring the Emergence Profile from the Provisional to the Final Restoration. Journal of Esthetic and Restorative Dentistry. 2013;26(3):154-161.
5. Castellon P, Casadaban M, Block MS. Techniques to Facilitate Provisionalization of Implant Restorations. Journal of Oral and Maxillofacial Surgery. 2005;63(9):72-79. doi:10.1016/j.joms.2005.05.152.
6. Yilmaz B, McGlumphy E. implant-supported fixed prosthesis. In: Rosenstiel S, Land M, Fujimoto J, ed., CONTEMPORARY FIXED PROSTHODONTICS, 5th ed. St. Louis: elsevier; 2016;342-345.
7. Stumpel J, Wadhwani C. A Customized Healing Abutment for Immediate and Delayed Implant Cases. Compendium of continuing education in dentistry. 2017;38(10):672-678.
8. Alshhrani W, Al-Amri M. Customized CAD-CAM healing abutment for delayed loaded implants. The Journal of Prosthetic Dentistry. 2016;116(2):176-179.
9. Finelle G, Lee, S. Guided Immediate Implant Placement with Wound Closure by Computer-Aided Design/Computer-Assisted Manufacture Sealing Socket Abutment: Case Report. The International Journal of Oral & Maxillofacial Implants, 2017;32(2):e63-e67.
10. Nkenke E, Fenner, M. Indications for immediate loading of implants and implant success. Clinical Oral Implants Research. 2006;17(S2):19-34.
11. Weber P, Morton D, Galluci O, et al. Consensus Statements and Recommended Clinical Procedures Regarding Optimizing Esthetic Outcomes in Implant Dentistry. The International Journal of Oral & Maxillofacial Implants 2009;24(Supplement):180-183.
12. Tarnow D, Chu S, Salama M, et al. Flapless Postextraction Socket Implant Placement in the Esthetic Zone: Part 1. The Effect of Bone Grafting and/or Provisional Restoration on Facial-Palatal Ridge Dimensional Change—A Retrospective Cohort Study. International Journal of Periodontics & Restorative Dentistry. 2014;34(3):323-331. doi:10.11607/prd.1821.
13. Garber D. The esthetic dental implant: Letting Restoration be the guide. The Journal of the American Dental Association. 1995;126(3):319-325.
14. Garber D, Belser, U. (1995). Restoration-driven implant placement with restoration-generated site development. Compendium of continuing education in dentistry. 1995;16:796-804
15. Lazzara J. Immediate implant placement into extraction sites: surgical and restorative advantages. International Journal of Periodontics and Restorative Dentistry. 1989;9(5): 332-343
16. Parel M, Triplett G. Immediate fixture placement: a treatment planning alternative. International journal of Oral and Maxillofacial Implants. 1990;5(4):337-345.
17. Wilson G, Schenk R, Buser D, et al. Implants placed in immediate extraction sites: a report of histologic and histometric analyses of human biopsies. International journal of Oral and Maxillofacial Implants. 1889;13(3):333-341.
18. Bahat O, Sullivan R. Parameters for Successful Implant Integration Revisited Part II: Algorithm for Immediate Loading Diagnostic Factors. Clinical Implant Dentistry and Related Research. 2009;12:e13-e22.
19. Esposito M, Grusovin G, Willings M, et al. The effectiveness of immediate, early, and conventional loading of dental implants: a Cochrane systematic review of randomized controlled clinical trials. International journal of Oral and Maxillofacial Implants. 2007;22: 893-904
20. Ottoni M, Oliveira F, Mansini R, et al. Correlation between placement torque and survival of single-tooth implants. International journal of Oral and Maxillofacial Implants, 2005;20:769–776.
21. Lemongello J.Customized provisional abutment and provisional restoration for an immediately-placed implant. Practical Procedures and Aesthetic Dentistry. 2007;19(7):419-424.
22. Yilmaz B, McGlumphy E. implant-supported fixed prosthesis. In: Rosenstiel S, Land M, Fujimoto J, ed; Contemporary Fixed Prosthodontics, 5th ed. St. Louis: elsevier;2016;334-340.
23. Mcrory ME, Cagna DR. A technique for fabricating single screw-retained implant-supported interim crowns in conjunction with implant surgery. The Journal of Prosthetic Dentistry. 2014;111(6):455-459. doi:10.1016/j.prosdent.2013.11.005.
24. Ganddini MR, Tallents RH, Ercoli C, Ganddini R. Technique for fabricating a cement-retained single-unit implant-supported provisional restoration in the esthetic zone. The Journal of Prosthetic Dentistry. 2005;94(3):296-298. doi:10.1016/j.prosdent.2005.06.010.
25. Vafiadis D, Goldstein G, Garber D, Lambrakos A, Kowalski B. Immediate Implant Placement of a Single Central Incisor Using a CAD/CAM Crown-Root Form Technique: Provisional to Final Restoration. Journal of Esthetic and Restorative Dentistry. 2016;29(1):13-21. doi:10.1111/jerd.12265.
26. Wang WC, Suzuki T. Utilization of extracted teeth as provisional restorations following immediate implant placement – A case report. Singapore Dental Journal. 2015;36:23-28. doi:10.1016/j.sdj.2015.10.001.
27. Margeas RC. Predictable Periimplant Gingival Esthetics: Use of the Natural Tooth as a Provisional following Implant Placement. Journal of Esthetic and Restorative Dentistry. 2006;18(1):5-12. doi:10.2310/6130.2006.00006.
28. Misch CM. Immediate loading of definitive implants in the edentulous mandible using a fixed provisional prosthesis: The denture conversion technique. Journal of Oral and Maxillofacial Surgery. 2004;62:106-115. doi:10.1016/j.joms.2004.06.042.
29. Kammeyer G, Proussaefs P, Lozada J. Conversion of a complete denture to a provisional implant-supported, screw-retained fixed prosthesis for immediate loading of a completely edentulous arch. The Journal of Prosthetic Dentistry. 2002;87(5):473-476. doi:10.1067/mpr.2002.123985.
30. David R. Provisional restoration for an osseointegrated single maxillary anterior implant. Journal of Canadian Dental Association. 2008;74(7):609-612.
31. Taylor TD, Agar JR, Vogiatzi T. Implant prosthodontics: current perspective and future directions. International journal of Oral and Maxillofacial Implants, 2000;15(1):66-75.
32. Kökat AM, Akça K. Fabrication of a screw-retained fixed provisional prosthesis supported by dental implants. The Journal of Prosthetic Dentistry. 2004;91(3):293-297. doi:10.1016/j.prosdent.2003.12.018.
33. Fradeani M. Creating and integrating the provisional restoration. In: fradeani M, Esthetic Rehabilitation in Fixed Prosthodonticts. quintessence publishing, 2008:130-188.
34. Buskin R, Salinas TJ. Transferring emergence profile created from the provisional to the definitive restoration. Practical Periodontics and Aesthetic Dentistry. 1998;10:1171-1179.
35. Ntounis A, Petropoulou A. A technique for managing and accurate registration of periimplant soft tissues. The Journal of Prosthetic Dentistry. 2010;104(4):276-279. doi:10.1016/s0022-3913(10)60139-4.