You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
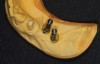
The use of dental implants as a treatment option has increased rapidly over recent years. Implant complications are usually the result of improper surgical placement (Figure 1). This can be reduced with the use of surgical guides for accurate and precise implant positioning to meet prosthodontic and esthetic requirements (Figure 2).1 Computed tomography, 3-dimensional implant planning software, and image and production techniques provide high accuracy in planning the angulation, orientation, and placement of implant fixtures. These crucial tools can help avoid misplacement, incorrect angulation, or iatrogenic damages in implant dentistry. Moreover, implant surgical guides help dentists to reduce implant placement time and effort, provide adequate information, and offer a more pleasant patient dental experience.2
Dental implant failures often arise as a result of lack of consideration of the exact placement site, accurate angulation, and proper examination of the surrounding structures during the planning stage. Accurate placement is mandatory to achieve the highest level of treatment quality either functionally or esthetically, as well as to achieve the highest level of patient satisfaction.3 This requires considerable collaboration among all members of the dental team, including the dental laboratory. The latter's involvement in the process is important so that a technician can offer their perspective. Making sure the laboratory is aware of all the clinical considerations assists in the fabrication process, as well.
The surgical implant guide helps to implement safe, minimally invasive surgical implant placement. The Glossary of Prosthodontics Terms defines "surgical guide" as a guide used to assist in proper surgical placement and angulation of dental implants.4 The main function of an implant surgical guide is to direct the drill in the correct and accurate direction according to the treatment plan.
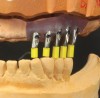
A surgical implant guide consists of two parts: the guiding cylinders and the contact surface. The contact surface fits either on an element of a patient's gingiva or on the patient's jaw. Cylinders within the drill guides help transfer the plan by guiding the drill in the exact location and orientation (Figure 3).5
Classifications
The surgical guides for implant placement can be classified in many different ways. In this article, two popular methods put forth by D'Souza and Aras6 will be discussed: classification based on fabrication design and classification based on the rest stop.
Classification based on fabrication design
There are three fabrication designs classified based on the amount of restriction offered by the surgical guide: non-limiting design, partially limiting design, and completely limiting design.
The non-limiting design only helps the dentist to indicate the planned prosthesis site. This design provides the ideal location of the implants without any guide to the angulation/orientation of the drill. Therefore, there is flexibility in the final positioning of the implant.
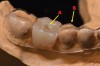
In a partially limiting design, the first drill used for the osteotomy (pilot drill) is directed using the surgical guide (Figure 4), and the remainder of the osteotomy and implant placement is then finished freehand by the surgeon. Techniques based on this design concept involve fabrication of a radiographic guide (Figure 5), after which the radiographic evaluation and verification can be converted into a surgical guide (Figure 6). Various authors have proposed different techniques involving modifications in the following stages of fabrication, such as the material used for the fabrication of the surgical template, radiographic marker used, type of imaging system used, and the conversion technique to convert the radiographic template into a surgical template.
Completely limiting design restricts the drill inside the bone in 3D vertical and horizontal directions (buccolingual, mesiodistal, depth of the preparation, and the positioning of the prosthetic table of the implant) (Figure 7). As the surgical guides become more restrictive, less of the decision making and/or subsequent surgical execution are done chairside. The completely limiting design includes two popular variations: cast-based-guided surgical guide and CAD/CAM-based surgical guide.
The cast-based-guided surgical guide technique is the combination of an analog technique done along with bone sounding and the use of periapical radiographs in a conventional flapless guided implant surgery.7 The periapical radiograph is rendered using a digital software for the transposition of the root structure onto the cast. The cast is then sectioned at the proposed implant site, and bone-sounding measurements are transferred to help the orientation of the drill to perform a cast osteotomy. Then, an implant analog is placed in the site, and a guide sleeve based on the implant width is modified using wires that are used to make a framework around the teeth.
The CAD/CAM-based surgical guide technology uses data from CBCT scans to plan implant placement. The CBCT images are converted into data that are recognized by imaging and planning software (Figure 8). The software then transfers this pre-surgical plan to the surgery site using 3D printing/milling technology (Figure 9 and Figure 10). The advantages of this technique include: the 3D views of the bone, which allow the dentist to visualize and evaluate length, width, and depth of the surgical site during treatment planning; and also avoiding the risks of exposing or invading the surrounding anatomic structures. This technique promotes flapless surgeries, allows pre-surgical construction of the master cast and provisional prostheses, and facilitates immediate loading. The accuracy of CAD/CAM technology in dental implant planning and predictable transfer of the pre-surgical plan to the surgical site has been studied.8 Verifying the implant placement and evaluating the implant orientation during guided surgery has been recommended by the literature.9,10 However, this technique also has its disadvantages, such as special training required for the dental team, as well as the possibility for inaccurate planning, radiographic stent error, and intrinsic errors during scanning, software planning, the rapid prototyping of the guide, and the transfer of information for the prosthetics.
Classification based on the rest stop
Aside from classification based on fabrication design, a surgical guide may also be classified based on its rest stop. When increased visibility is needed in partially or fully edentulous cases, bone-supported guides are developed. Mucosa-supported fabrications are often used in fully edentulous cases when minimally invasive surgery is preferred (Figure 11). When minimally invasive surgery is preferred for single-tooth and partially edentulous cases (Figure 4), tooth-supported guides are recommended.5
Interdisciplinary Approach to Surgical Guide Fabrication
Like any other aspect of implant dentistry (ie, diagnosis, treatment planning, and treatment execution), fabricating surgical guides for implant placement should also be considered with an interdisciplinary approach. The restorative dentist, in conjunction with the dental laboratory, should evaluate the radiographic guide and the CBCT scan before fabricating the surgical guide (Figure 12 through Figure 14). Often, the dental laboratory proposes implant placement, orientation, and angulation while planning, which ultimately requires a practicing dentist to approve prior to fabrication of a surgical guide. Having an interdisciplinary approach, which includes surgeon, dentist, and laboratory, provides for the best treatment outcomes. The laboratory's input is based on restorative considerations and expected outcomes, while the surgeon contributes to optimize those surgical outcomes by explaining the limitations and challenges of the implant placement phase. This is because placing an implant exactly where the diagnostic wax-up dictates may not always lead to a predictable surgical outcome considering the anatomic and biological limitations (Figure 15). Hence, the surgeon, restorative dentist, and laboratory should always approach these cases with plenty of communication, since the prognosis of implant-supported/-retained prostheses and the implant fixtures are intertwined.
Acknowledgement:
The authors would like to acknowledge Steven Pigliacelli, MDT, CDT, Marotta Dental Studio, NY, for providing some of the figures.
About the Authors
Siamak Najafi-Abrandabadi, DDS
Clinical Assistant Professor, Department of Prosthodontics
NYU College of Dentistry
New York, NY
Hesham Alouthah, DDS
Advanced Programs for International Dentists in Comprehensive Dentistry
NYU College of Dentistry
New York, NY
Niloufar Amintavakoli, DDS, MSc, FRCD (C)
Clinical Assistant Professor, Department of Oral and Maxillofacial Pathology, Radiology & Medicine
NYU College of Dentistry
New York, NY
References
1. Ganz SD. Presurgical planning with CT-derived fabrication of surgical guides. J Oral Maxillofac Surg. 2005;63:59-71.
2. Garber DA, Belser UC. Restoration-driven implant placement with restoration-generated site development. Compend Contin Educ Dent. 1995;16:798-804.
3. Widmann G, Bale RJ. Accuracy in computeraided implant surgery: A review. Int J Oral Maxillofac Implants 2006;21:305-13.
4. Ferro KJ, et al. The glossary of prosthodontic terms: Ninth edition. J Prosthet Dent. 2017;117(5S):e1-e105.
5. Ramasamy M, Giri, Raja R, Subramonian, Karthik, Narendrakumar R. Implant surgical guides: From the past to the present.J Pharm Bioall Sci. 2013;5:98-102.
6. D'Souza KM, Aras MA. Types of implant surgical guides in dentistry: A Review. J Oral Implantology. 2012;38(5):643-652.
7. Stumpel LJ 3rd. Cast-based guided implant placement: a novel technique. J Prosthet Dent. 2008;100:61-9.
8. Zhou W, Liu Z, Song L, Kuo CL, Shafer DM. Clinical Factors Affecting the Accuracy of Guided Implant Surgery-A Systematic Review and Meta-analysis. J Evid Based Dent Pract. 2018;18(1):28-40.
9. Marliere DAA, Demetrio MS, Picinini LS, De Oliveira RG, Chaves Netto HDM. Accuracy of computer-guided surgery for dental implant placement in fully edentulous patients: A systematic review. Eur J Dent. 2018;12(1):153-160.
10. Seo C, Juodzbalys G. Accuracy of Guided Surgery via Stereolithographic Mucosa-Supported Surgical Guide in Implant Surgery for Edentulous Patient: a Systematic Review. J Oral Maxillofac Res. 2018:31;9(1):e1.