You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
New computer-aided design and computer-aided manufacturing (CAD/CAM) systems are quickly being introduced to the market. With each release, technology becomes more precise and reliable. As technology continues to improve and become more efficient than humans in certain areas, some in dentistry may grapple with the ramifications of the long-term impact. Technology has changed the landscape of dentistry; however, a machine can never replace unique human abilities. It can make our lives easier by simplifying the processes that we use and leveraging valuable time. But first, we must learn how to best use these advancements.
Leverage Our Efforts
With all these changes comes the need for new protocols and procedures for both the clinical side and laboratory. These digital tools were made to simplify processes. Because these products are proliferating dental offices and laboratories, dentists and dental technicians are learning to change their ways of practice.
Especially being affected are the full-mouth implant-supported restorations that we are now able to offer patients. New software and materials, as well as improvements in old materials, make the systems more predictable and precise and also require learning to be a constant need for both the dentist and dental technician. This includes new ways of communicating with all team members involved. Dentists and technicians are asking patients to invest in their expertise; so dental professionals are obligated to know which product is the best for each case, how the product will function, what its limitations are, and what the correct preparation design should be. Then dentists should ask technicians what is the best and most efficient way to successfully convey all the information in the patient’s mouth to the laboratory. Without these steps, a practice may not have satisfied patients or esthetic restorations.
Equally important is emphasizing with patients that technology is only a small part and an “enhancement” of the dentist’s personal service. It is still the human touch, a clear vision of the final outcome, effective collaboration, and emotional intelligence that makes the biggest difference for the patient.
The Current State of Digital Dentistry
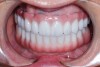
As advancements are made in digital procedures and new materials emerge to complement these processes, it seems that our standards for what is considered acceptable have declined (Figure 1). Poorly executed dentistry is seen all too often. The same norms for esthetics that we once fought to improve in the 1970s are now “good enough” because a machine made them. Machines can make our lives easier; however, machines are about 80% of the work of the dental technician, but it’s 20% of the human touch that makes 100% of the difference with patients.1 But that 20% now is accomplished in different ways and possibly a little harder to achieve. Time must be made to learn these new procedures by all involved. Constant and continuous improvement is what makes any profession great, and dentistry is certainly no exception. Our minds, experiences, the care, and responsibility that we have for our patients, as well as each technician’s unique talents, play the largest role, even in CAD/CAM dentistry.
Plastic vs. Zirconia Screw-Retained Prosthesis
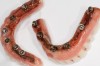
Denture teeth are beautiful. If they are set properly, the smile of a patient with edentulism can be beautifully restored with a plastic prosthesis.2 However, one of the latest players in the dental arena is the implant-supported zirconia hybrid denture. But, even for some, it seems that this has been another reason to say “good enough” in regard to esthetics and function. A plethora of zirconia hybrids that do not resemble natural teeth or tissue have bombarded the market.1 However, these zirconia hybrids are worth investing time to learn to implement because they solve a number of problems that plastic hybrid dentures have: denture teeth that “pop off” because of the rigidity and strong forces, discoloration of the plastic, odors that the plastic retains, loss of vertical dimension with time, debonding from the bar, and cracking (Figure 2).1
Working with zirconia restorations is technique sensitive,3 and each step in fabricating these restorations is equally as important. The scan, computer design, green-stage manipulation of shading and shaping, milling of the zirconia, and ceramic touches of the pink layers all need the human touch for the final product to appear natural. Milling machines on the market are similar in that the device itself does not make much difference in whether the restoration looks natural. Much like a dentist’s handpieces, many similar milling devices are on the market, but the outcome of a tooth preparation is totally dependent on the skill and knowledge of the operator, not just the equipment. The same is true with CAD/CAM technology. Each laboratory technician has unique skills and talents. However, the individual’s vision is what makes the difference, not the machine. The only reason that unnatural CAD/CAM restorations are abundant is because the human touch has been omitted.1
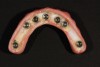
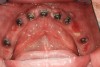
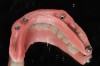
This article will illustrate this point using treatment with a full-arch implant-supported zirconia restoration as an example. The importance and the critical factors are: gaining and maintaining health of the tissue by having an intaglio surface that is easily cleanable (without this, failure is inevitable)4 (Figure 3 and Figure 4); and beautiful, natural esthetics that mimic nature (Figure 5).
The Exacts
Through research and study, different processes have been developed that make life easier and more predictable while saving time for the dentist, patient, and technician. The dental industry is constantly changing, and the traditional models do not work as they used to. Plastic screw-retained dentures have lost their appeal, and their zirconia counterparts, which present more esthetic and longer-lasting results, are quickly taking their place in the market.1
The days of compromising on the esthetics of zirconia are gone. Strength and longevity no longer have to come with lifeless esthetics.5 For a successful long-term zirconia hybrid restoration,6 the vertical height measured from the margin of the non-engaging abutment to the occlusal of the tooth in the posterior area must be 12 mm to 15 mm, (Figure 6); anything less will cause the zirconia to break. Planning at the surgical phase, prior to implant placement, is of special importance to ensure the proper height. The bone must be reduced sufficiently to ensure that a ridge lap can be avoided.7
The Intaglio Surface
Long-term health and longevity of the implants rely highly on, among other things, having the proper intaglio surface. The ridge-lap design should be avoided. Even though zirconia is highly conducive to healthy tissue, if a ridge-lap design is made, cleaning is not predictable, as shown in Figure 3 and Figure 4. The tissue is not healthy, and mucositis, bleeding, calculus, and food can be detected. In a case in which a ridge-lap design must be done, a removable type of denture would be better for ease of removal and cleaning.6
All-in-One Process
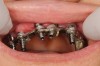
Traditionally, a jig for verification is needed to ensure the accuracy of the master model and the titanium cylinders will be cemented for the final case. These traditional jigs are usually made from a durable or composite material that connects the impression copings and is reinforced with floss. After the material has set, the dentist traditionally sections the jig, replaces it back into the mouth, and then reconnects it with more material to minimize the shrinkage. This process is time consuming and not accurate for zirconia because zirconia is much more rigid and the acrylic/composite does flex. Any discrepancy could cause a fracture to the zirconia prosthesis. The author has found an easier and more predictable way to get the same information to the laboratory with an all-in-one process.
Premeasured metal bars vary in length, with premilled holes at both ends that fit over either impression copings or non-engaging abutments. A tool is provided for measuring the length needed. Once these metal bars are seated, they can be connected with either a light-cured or self-curing resin in generous amounts to ensure that movement is not possible (Figure 7). An option for a patient who has remaining existing teeth is to take an open-tray impression over the premeasured bars that have been luted into place and send that to the laboratory for fabricating an accurate master model. For a full-arch edentulous case, a flowable temporary type of material can be syringed under and over the premeasured bar, encasing the bar and capturing the impression of the tissue underneath. The bar impression is then unscrewed from the mouth and sent to the laboratory.8
To ensure no shrinkage of the master models occurs, the laboratory will connect laboratory analogs to the impression (Figure 8) by injecting soft-tissue material first and then placing the bars and connecting with either a light-cured or acrylic resin (Figure 9). This is also to ensure no breakage occurs if the model is dropped (Figure 10). These bars also ensure that trimming the abutments will not disturb the model or destroy the plaster and lessen distortion, thereby increasing the accuracy.
The author has found performing these two steps correctly will provide the dentist with 99% accuracy of the restoration and master model.1
Duplicating the Denture
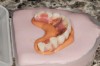
Another way to be more effective and save the patient money is to duplicate the prosthesis instead of having an extra made for a wax-up try-in for esthetic reasons. The author has found a better and more predictable way to obtain the information regarding the patient’s current denture, which entails taking a precise impression, in a specific manner, of the occlusal side and intaglio surface of the prosthetic, thus rendering the need for a secondary denture unnecessary (Figure 11 and Figure 12). This new two-step technique is predictable by using a retainer-type case holder, mixing a hard-body impression material, and using a light-body wash squeezed in the intaglio surface of the denture. After it is set, a lubricant should be put on all surfaces of the impression and retainer top. It should be sandwiched together, and rubber bands should be used to ensure adequate closing of the retainer case. Once it has set, the silicone parts should be carefully separated, and the denture can be removed and returned to the patient. The dentist now has an accurate impression of the denture that can be sent to the laboratory, which will become a reference point to modify either by shaping (Figure 13) in wax or digitally after scanning for fabrication of polymethyl methacrylate (PMMA).
Polymethyl Methacrylate
The use of PMMA is the most crucial step in the zirconia hybrid process (Figure 14). PMMA is a tool employed to decide every determining factor that will make the prosthesis a success.9 The laboratory needs specific pictures of reference points of the denture in the patient’s mouth: full-facial view with the patient smiling, close-up smile, profile smile (both sides), retracted photo of the converted denture in the mouth, and retracted perspective of the implants.
This is the stage when the intaglio-surface design needs to be determined to make sure the patient is able to floss and use a water flosser to clean the surface beneath the restoration. It is a three-dimensional restoration that the patient will wear to determine the design for optimal tissue health, proper function and occlusion, and esthetics. Once everything is confirmed in the PMMA stage, the final zirconia prosthesis should be executed. The tissue should be healed, the occlusion completely adjusted, and the esthetics confirmed; only then should the zirconia prosthesis be done. Once the PMMA is scanned and zirconia is milled, no changes should be made to the zirconia, as it will never be as polished as it is after leaving the ceramic oven. Nothing manual will ever reproduce that, and so bacteria will adhere and make cleaning the intaglio surface hard, if not impossible to do. Not to mention the fact that trimming zirconia is difficult and the overheating created by it could cause breakage or microfractures that may only show themselves after the patient has been wearing the restoration.6
The Green Stage
Now that the occlusion, midline, shape, and esthetics have been finalized in the PMMA stage, it is time for the most crucial step in fabricating the full-monolithic zirconia prosthesis—the green stage. This is when the major difference between one laboratory and another happens. The prosthesis in the green stage is 20% larger than the final prosthesis will be and is very soft (Figure 15). This gives the technician the ability to create definition, texture, shape, and color—when the “human touch” starts. The green stage is also when breakage is much more likely, so care must be given to not chip a margin, as the entire process must be restarted. Once the green stage is sintered in the oven, the wax should not be touched to avoid the risk for creating microcracks from overheating.6 The shaping in the green stage is important to make “believable” esthetics. There are specific tools on the market to enhance the shape.6
Once it has been trimmed, the coloring process begins. Most zirconia blocks are available in one shade—bright—so any detail and enhancement of esthetics must be done in the green stage. The softness of the green stage allows the stains to infiltrate the zirconia and is the only time that color can be added internally (Figure 16). After sintering, only surface stains can be added, but the restoration will not look like natural teeth unless stains are used on the green stage prior to sintering.
To Layer or Not to Layer
Zirconia is known for its strength and is perfect for people who destroy restorations through clenching and bruxism. However many technicians cut zirconia back to layer in porcelain to enhance the esthetics of the bright and “dead-looking” material, leaving only the base of zirconia. This completely removes the strength of zirconia. In studies at the author’s laboratory, the author has found even with minimal cutback on nonfunctional areas only, some patients still manage to sheer the ceramic. The author also determined if the porcelain can be repaired, the patient will break it again quickly in most cases.6 Hybrid-wearing patients who have lost their teeth tend to lose proprioception no matter how well the occlusion has been adjusted, making the risk for breakage high.6
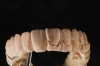
Full-monolithic zirconia is more difficult to make natural and lifelike but is definitely possible to do (Figure 17). Having a clear vision of the outcome and spending adequate time in the green stage shaping and creating definition while preserving the strength of the material is necessary. Some effects can be done after sintering using 3D stains specifically for this purpose. These stains create a silky finish and enhance the effects.
Minimally layered and full-monolithic zirconia can be hard to detect when these methods are followed. Full-monolithic zirconia looks as good as layered, is less costly to the patient and dentist, is stronger, and will not chip (Figure 18). The philosophy at the author’s laboratory is to devote more time in the green stage to maximize the illusion of reality to create natural-looking full-monolithic restorations.
Summary
The key to success is to involve all dental professionals at the beginning of treatment planning.9 Providing all team members with diagnostic records and detailed reports on the current situation, including facial shape;10 dimensions; dentition occlusion; bone and soft-tissue topography; and distinctions in the existing smile, are all pieces of information necessary for success and to help eliminate the chance for challenges.11
Full-monolithic zirconia restorations have greater wear resistance and are extremely biocompatible for soft tissue. Abuse or inappropriate use of the product will lead to failure either during production or after delivery. We should not blame the material, only the operators.
Like-minded team members who understand the patient’s needs and desires and are able to communicate with them effectively are of utmost importance.
Becoming complacent with technology and accepting “good enough” is never the answer. It is the laboratory technician’s artistic responsibility to bring life to these machined restorations and treat machines as a tool and not a panacea. It is the common vision, values, and collaborative effort of the entire dental team that will create the recipe for success (Figure 19).
Acknowledgments
A special thank-you to the collaborating clinicians who believe in high-quality dentistry, fight mediocrity, and become a part of the team at Adar Dental Laboratory in sharing what is possible in CAD/CAM digital dentistry. The author thanks Dr. Sanjeev Goel of West Chester, OH, for Figures 2, 3, 8 through 13, and 16 through 18, and Dr. John Heimke of Rocky River, OH, for Figures 6, 14, 15, 19, and 20. Special thanks also to Enrico Steiger, Zirkonzahn International; Alessandro Cucchiaro and Katana Uonkaen of Zirkonzahn, Atlanta, GA; and Ash Michalec, Luc Tendron, and Debby Adar of Adar Dental Laboratory, Atlanta.
About the Author
Pinhas Adar, MDT, CDT
Adar Dental Network, Inc
Atlanta, GA
References
1. Adar P. Incorporating the human touch in restorative outcomes. Inside Dent Technol. 2014;5(12):52-56.
2. Patil SB, Naveen BH, Patil NP. Bonding acrylic teeth to acrylic resin denture bases: a review. Gerodontology. 2006;23(3):131-139.
3. Raigrodski A. Managing prosthetic challenges with a CAD/CAM zirconia restoration. J Cosmetic Dent. 2014;30(2):40-52.
4. Lang NP, Tonetti MS. Peri-implantitis: etiology, pathogenesis, prevention, and therapy. In: Froum SJ, ed. Dental Implant Complications. Chichester, West Sussex, United Kingdom: Wiley-Blackwell; 2010.
5. Rojas-Vizcaya F. Full zirconia fixed detachable implant-retained restorations manufactured from monolithic zirconia: clinical report after two years in service. J Prosthodont. 2011;20(7):570-576.
6. Adar P, Pearson C. The proof is in the laboratory; comparison of maxillary full-arch implant supported zirconia. J Cosmetic Dent. 2015;31(1).
7. Rutkunas V, Ignatovic J. A technique to splint and verify the accuracy of implant impression copings with light-polymerizing acrylic resin. J Prosthet Dent. 2014;111(3):254-256.
8. Zinner ID, Markovits S, Jansen CE, et al. Sequential provisional implant prosthodontics therapy. Gen Dent. 2012;60(6):508-518.
9. Adar P. Communication: the ultimate in synergy. Inside Dent. 2005;1(1):82-83.
10. Nold SL, Horvath SD, Stampf S, Blatz MB. Analysis of select facial and dental esthetic parameters. Int J Periodontics Restorative Dent. 2014;34(5):622-629.
11. Papaspyridakos P, Lal K. Computer-assisted design/computer-assisted manufacturing zirconia implant fixed complete prostheses: clinical results and technical complications up to 4 years of function. Clin Oral Implant Res. 2013;24(6):659-665.