You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
With the plethora of new products becoming available, material selection can make a significant difference. The authors have found one particular product that helps them handle full-arch fixed removable cases more effectively and efficiently than ever.
Treatment Planning
In this case, the laboratory was tasked with fabricating a screw-retained full-arch upper denture over an opposing cement-retained full-arch lower denture. The laboratory recommended to the dentist that the substructures be fabricated with TRINIA™ (Shofu Dental Corporation, shofu.com), a biocompatible, metal-free material that has high flexural and compressive strength to facilitate intraoral comfort and function.
TRINIA’s durability and resiliency can be attributed to its multi-directional, interlacing layers of fiberglass and resin. The material is available in round or D-shaped pucks as well as two different block sizes. It can be precisely and efficiently milled on many leading wet or dry milling machines with nano-diamond or carbide burs, unlike titanium substructures, which generally must be sent out for milling by a third party. With TRINIA, there is no risk of distortion, which can occur with substructures milled in semi-precious or precious metals. TRINIA substructures are also readily adjustable with a standard carbide bur and can be given a high gloss shine using a composite polishing protocol. The unit cost for these substructures is far less than the cost of those that use semi-precious metals, precious metals, or titanium. The dentist agreed with the recommendation to fabricate the substructures with TRINIA, and the case proceeded.
Laboratory Process
The models were poured with the appropriate analogs in place, soft tissue placed around the analogs, bite rims prepared, and records taken. Upper and lower try-ins were fabricated and sent out for patient approval.
Once the approved try-ins were returned, the next step was to scan the try-ins on the casts. The try-ins and soft tissue were then removed, the scan jigs were attached, and the models were scanned with and without the soft tissue in place. The purpose of these scans was to create files that would be used to design substructures fitting within the parameters of the try-ins.
The bars were designed utilizing CAD software and sent to the milling machine. In this case, the pink, round TRINIA puck was chosen because the puck shape fit the milling machine being used. The pink color was selected to match the tissue color of the processed acrylic so that no masking would be required to disguise the substructures.
The try-ins were returned to the models without the substructures in place. Silicone indices were fabricated to hold the position of the teeth once the wax was removed (Figure 1). The silicone indices were taken off the models, the wax was removed, and the teeth were returned to the indices using a tiny dot of adhesive on each tooth to affix it securely.
Because the upper appliance would be screw-retained, it was preferable to use titanium bases for metal-to-metal contact between the implants and the substructure. The titanium bases were prepared by sandblasting the outside of the bases and then painting the outside of the bases with a metal primer (ML Primer, Shofu Dental Corporation). The titanium bases were screwed into place on the upper cast without the soft tissue.
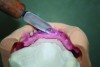
Next, the upper substructure was prepared to receive the titanium bases. The intaglios of the substructure were sandblasted, steam-cleaned, and wiped with a cotton swab with alcohol. A thin coat of Ceraresin Bond 1 (Shofu Dental Corporation) was applied to each intaglio and allowed to dry for 1 minute. A light coat of Ceraresin Bond 2 was applied to each intaglio and then the substructure was light-cured for 3 minutes. A small, even coat of cement (MonoCem, Shofu Dental Corporation) was placed on the surface of each titanium base and then the upper substructure was affixed on top of the titanium bases, maintaining pressure for 3 minutes to set the cement (Figure 2).
The upper substructure was then unscrewed from the cast with the titanium bases securely affixed. The soft tissue was returned to the cast and the substructure was reattached to the cast to check for any premature contacts between the soft tissue and the substructure. The fit of the lower substructure with soft tissue was likewise confirmed on the lower cast; however, titanium bases were not needed on the lower as this substructure was to be cemented directly to the abutments. After the fit of the substructures was verified, the silicone indices were placed back on the casts and the teeth were luted in place (Figure 3). The upper and lower were waxed up for a final try-in, making certain that the access holes on the upper were kept clear of any wax or debris.
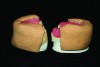
The case was sent out for a try-in and upon return, necessary adjustments were made. The upper was invested using the standard full-arch fixed protocol for processing, utilizing analogs to fabricate a processing cast (making sure that the access holes were blocked out). Alternatively, the try-in with analogs could be placed directly into the lower half of a flask and invested. The lower was invested directly into a flask, but because analogs were not readily available, they were created with a very low fusing metal and paper clips were used for retention. These analogs on the lower kept the substructure in position after boilout and during processing (Figure 4). The upper and lower were cured overnight at 163°F with a high-impact acrylic and then bench cooled. The dentures were then finished and naturalized with Ceramage Gum Color Composites (Shofu Dental Corporation) to further enhance the esthetics of the finished appliances.
The dentures were polished and remounted on the original casts. The occlusion was verified and adjusted as needed. The case was delivered to the dentist along with appliance care instructions for the patient (Figure 5).
Conclusion
TRINIA is gaining attention as an exceptional metal-free alternative for substructures. The material is biocompatible, lightweight, and yet extremely durable. It is far more economical than other substructure choices. The fact that it can be milled on most leading milling machines means that the work generally can be done in-house with substantial savings in turnaround time.
About the Authors
Jim Collis, CDT
Owner of Collis Prosthodontic Laboratory
Elmhurst, IL
Jeffrey Slovick, DDS
Private Practice
Elmhurst, Illinois