You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
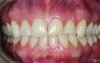
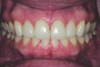
A 37-year-old woman who had been in the practice since childhood expressed interest in improving the appearance of her front teeth (Figure 1). Her main concern was lower anterior crowding. She had no history of orthodontic treatment. Her medical history was non-remarkable, and she was classified as ASA1.
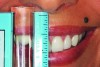
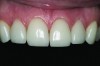
The patient’s dental history included a recent history of cracked teeth and a complaint that her teeth seem to be getting shorter (Figure 2). She also reported that she had “more than one bite,” and felt that the lower anterior crowding seemed to be getting worse. She had whitened her teeth with no adverse effects.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: This patient had maintained a very consistent schedule of 6-month recalls since childhood. There were several 4-mm pockets in the posterior, with all other areas measuring 3 mm or less. No bone loss of greater than 2 mm was evident on the full-mouth radiographic series. No evidence of mobility was noted. Tooth No. 10 had a 1-mm area of recession. She was determined to have AAP Type 2 mild adult periodontitis. Risk: Low. Prognosis: Good.
Biomechanical: Tooth No. 3 had a defective distal-occlusal-lingual onlay and active caries on the mesial. Tooth No. 30 had an enamel lesion on the mesial that radiographically did not appear to have penetrated the dento-enamel junction. When prior radiographs were reviewed, it was noted that the appearance was unchanged over time. Teeth Nos. 3, 14, and 18 were deemed to be at risk for future endodontic treatment due to the presence of full-coverage restorations on teeth Nos. 14 and 18 and the large defective restoration, and caries on tooth No. 3. Tooth No. 15 had a questionable occlusal composite restoration. Incisal erosion was evident on teeth Nos. 7 through 10 and 23 through 26. Attrition was evident on teeth Nos. 7, 9, and 10. Teeth Nos. 9 and 10 had been restored 19 years previously after an accident, and the restorative material also displayed attrition.
Risk: Moderate.
Prognosis: Generally fair; hopeless for tooth No. 3 without caries treatment.
Functional: The patient reported “having more than one bite” on the dental history evaluation. She reported no TMJ symptoms, and the clinical evaluation of the temporomandibular joints revealed no pain, soreness, or joint sounds. The load and immobility tests were normal and her opening was 54 mm with no deviation. Abnormal attrition was noted on teeth Nos. 7, 9, and 10. After wearing an anterior deprogrammer, the point of initial contact was on posterior teeth Nos. 2 and 31, confirming the diagnosis of occlusal dysfunction.
Risk: Moderate.
Prognosis: Fair.
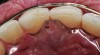
Dentofacial: With an unguarded smile, the patient had bilateral display of her teeth, gingiva, and interdental papillae posteriorly to the first molar (Figure 3). She also showed approximately half of her lower incisors with a wide “eee” smile. In repose, the maxillary canines were at a 0 position relative to the resting lip, and the movement of her upper lip when she smiled was hypermobile (Figure 4 and Figure 5).
Risk: High.
Prognosis: Fair.
Treatment Plan Presentation and Informed Consent
At the treatment plan presentation, the patient agreed to treatment to restore the proper length of the upper incisors, but she rejected orthodontic treatment to address the lower anterior crowding. She also accepted treatment of the four maxillary incisors after viewing a laboratory wax-up and understanding the esthetic outcome that could be achieved with porcelain veneers. An alternative proposal was offered to mask the mandibular crowding with enamoplasty and direct composite restorations for the lower incisors. She was informed that this was a compromise relative to orthodontic treatment, and she agreed to complete the maxillary restorative treatment prior to the enamoplasty of the lower incisors.
Treatment Goals
The following specific measures were established as treatment goals: Treat the occlusal dysfunction with equilibration, and avoid creating a constricted chewing pattern after the equilibration. Treat the caries and defective restoration on tooth No. 3 with an indirect porcelain onlay. Restore the appropriate incisal length of teeth Nos. 7 through 10 with feldspathic porcelain veneers. Close the space between teeth Nos. 10 and 11 while maintaining harmonious mesiodistal proportions with direct composite bonding on the mesial of tooth No. 11. Resolve lower anterior crowding orthodontically. (The patient initially refused this treatment, but she changed her mind after the veneer treatment was completed.) Maintain periodontal health with a continued 6-month recare schedule. Provide instruction to maximize potential for continued stability of the arrested lesion on tooth No. 30.
Treatment Sequence
Phase 1—Establishment of Centric Relation
Prior to any restorative care, the patient wore a Kois deprogrammer1 (Figure 6). Once the deprogramming was confirmed, the models were mounted in centric relation (CR).
A trial equilibration was performed on the mounted models to verify that the equilibration could be performed without undue tooth structure removal and without causing a constriction in the anterior. The occlusal equilibration was then completed intraorally to an acceptable endpoint with simultaneous bilateral equal contact in the posterior teeth and no anterior contact in the envelope of function.
Phase 2—Models Created, Mounted in MIP, and Evaluated
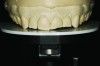
After the equilibration was completed, new alginate impressions were made, and then poured in stone for mounting, esthetic evaluation, and wax-up. The stone models were inspected for any distortions and trimmed for mounting. A facebow record was taken with the Kois Dento-Facial Analyzer System (Panadent, panadent.com) to accurately position the maxillary cast on the articulator with the platform and incisal pin set at 0 (Figure 7). The maxillary cast was then mounted onto the articulator using the removable plate from the facebow (Figure 8). Because the patient’s occlusal dysfunction was successfully treated with the occlusal equilibration, the models could be mounted in maximum intercuspal position (MIP), which after treatment to an acceptable function was coincident with CR.2,3
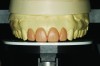
After evaluation of the mounted models, it was decided that tooth No. 8 was at the appropriate incisal length4 (Figure 9). If it had been determined that a different incisal length was necessary, the articulator platform could have been moved to the appropriate position with the wax-up, then guided by the platform position. In this case, the wax-up was done to the desired length by simply waxing to the zeroed platform and incisal pin (Figure 10). Teeth Nos. 7 through 10 were waxed up to give pleasant symmetry to the provisional and final restorations. Serving as a model for final restorations, the wax-up was used to fabricate Luxatemp® (DMG, dmg-dental.com) provisional restorations for an esthetic and functional trial.
Phase 3—Restoration Placement
After the diagnosis and treatment plan was completed using standard protocols, an enamel- supported mesio-occlusal-distal-lingual feldspathic porcelain onlay was placed to treat the carious lesion and defective existing restoration. Feldspathic porcelain veneers were placed on teeth Nos. 7 through 10 using standard protocols, and a small direct composite restoration was bonded to the mesial of tooth No. 11 to maintain the correct size proportions of the maxillary anterior teeth. Because the canines were not involved in the treatment plan, the acceptable function established previously with the occlusal equilibration was not compromised or altered. A satisfactory esthetic and occlusal result was obtained (Figure 11).
Phase 4—Orthodonture
After the veneer treatment was finished, the patient decided that she did indeed want to have limited orthodontic treatment to resolve the lower anterior crowding. Referral to an orthodontist and a short course of limited orthodontics quickly and conservatively addressed the patient’s presenting concern.
Discussion and Conclusion
While initially reluctant to pursue orthodontics to solve her chief concern, the patient was willing to address her maxillary teeth. Once this treatment was completed, she opted for correct positioning of her lower anterior teeth instead of the compromise approach4 enamoplasty. She had an excellent result (Figure 12). Her periodontal risk remains low, with a good prognosis, and she remains on a 6-month recall.
Biomechanically, the prognosis was improved from hopeless to fair for tooth No. 3 because active caries were treated. Enamel surface management for the arrested lesion on tooth No. 30 included patient education to minimize risk of lesion progression. Enamel-supported veneers on teeth Nos. 7 through 10 did not substantially increase the risk to these teeth.
The functional risk was lowered from moderate to low and she now has stable, acceptable function. The occlusal equilibration successfully addressed the diagnosis of occlusal dysfunction. She now reports stable function. The position of the anterior teeth does not impinge on the envelope of function. By addressing the occlusion first, all treatment provided continued to maintain acceptable function throughout the restoration and orthodonture in both arches. The patient was extremely happy with all of her definitive restorations and that her lower anterior crowding was successfully treated with orthodontics.
The patient’s dentofacial risk remained unchanged, as no treatment (Botox, lip lengthening) was provided to address the amount of gingival display due to her high lip line. The patient expressed no concerns, either preoperative or postoperative, about the gingival display when she smiled. Her prognosis did improve because the maxillary anterior teeth were restored to harmonious proportions and length, and her mandibular anteriors were no longer visibly crowded and rotated (Figure 13 and Figure 14).
References
1. Jayne D. A deprogrammer for occlusal analysis and simplified accurate mounting. J Cosmetic Dent. 2006;21(4):96-102.
2. Kois J, Hartrick N. Functional occlusion: science-driven management. J Cosmetic Dent. 2007;23(3):54-57.
3. Dawson PE. Centric relation. Its effect on occluso-muscle harmony. Dent Clin North Am. 1979;23(2):169-180.
4. Misch CE. Guidelines for maxillary edge position-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
Acknowledgments
The author would like to thank Erik Southers, DDS, for providing the orthodontic care in this case, and Nelson Rego, CDT, for his expert laboratory work.
Disclosure
The author had no disclosures to report.
About the Author
John Scalas, DDS
Private Practice
Cypress, California