You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
The book The Second Machine Age separates the concepts of physical investment and human capital in the workplace. Physical investment in the production of dental prosthetics includes many processes digitized through the development of and investment in machines producing single crowns to complete dentures. Human capital, conversely, involves processes that cannot be accomplished by digitization. Providing complete denture service in planning in preparation for a full-arch implant-supported prosthesis requires the human eye and artistic sense to select appropriate denture teeth and manipulate baseplate wax on record bases, as well as the hands-on and interpersonal skills to interact with patients in a clinical setting that cannot be duplicated with a computerized process. These include the initial steps necessary to provide segmental implant-supported prosthetics as well as complete dentures, partial dentures, and fixed restorations supported by natural teeth.
Dental schools have been moving from teaching predoctoral dental students the skills and broad experience necessary to provide complete denture service. Why should educators waste time teaching such an undervalued service when dentists can make one implant-supported crown at the same price as a complete denture? Some suggest that educating dentists to provide this service is the responsibility of dental technicians. However, administrators, faculty, and curriculum committees in many cases do not understand and appreciate the value of complete denture service or how to charge a proper fee for that service.
Analog methods to define required lip support and reestablish normal appearance utilize a record base with baseplate wax. Computerized processes cannot duplicate these procedures because interpretation of several factors is required, including lip support, lip mobility within the lip frame, and a volume change below the facial muscles. Several key considerations critical to the success of complete denture service require human clinical/technical skill and interpretation.
Lip Support
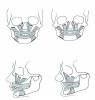
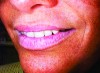
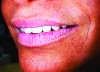
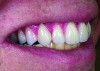
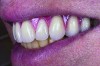
Often when teeth are lost as a result of periodontal disease, tooth decay, or traumatic injury, alveolar bone that houses teeth is lost. Particularly in the maxillary arch, bone loss moves the bony scaffolding supporting the facial muscles medially, posteriorly, and superiorly, causing loss of lip support and eversion. Figure 1 and Figure 2 illustrate the inward collapse of the face when the bone and teeth are lost.
Baseplate wax on a record base is hand molded, formed with a flat heated spatula, modified, and tried in the patient’s mouth to develop the support necessary to replace what has been lost. The lower edge of the upper wax rim is adjusted to contact the wet dry line of the lower lip while the bulk of the wax rim should create adequate scaffolding to replace the lost bone and tooth support into the buccal corridor. The width of the baseplate wax varies, reflecting the volume of space that will be occupied with the prosthetic teeth — wide in the posterior area and thin at the incisal edges of the anterior teeth.
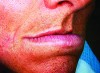
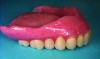
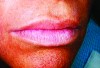
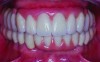
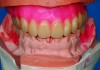
Figure 3 illustrates severe bone loss in the upper arch in a patient who has been edentulous for 20 years. The profile of the wax rim when viewed from the side may have two planes, with one from the angled reflection of the buccal vestibule and the second representing the location of the denture teeth. Often these two planes are necessary to provide the missing volume of alveolar bone and support for the superior aspect of the upper lip. In the completed denture (Figure 4), the two planes meet from cuspid to cuspid at the gingival line where the denture base meets the denture teeth supporting the upper border of the upper lip. Figure 5 demonstrates the effect of the required volume provided by the denture base and denture teeth to support and restore the desired appearance.
Phonetics
A key function of anterior teeth is to facilitate clear speech and natural appearance. Each patient has a specific mandibular movement and position during speech, a function that cannot be recreated using a non-specific computer model. Earl Pound, DDS, suggested that mandibular movement during speech is related to neuromuscular memory that the patient with edentulism used during speech with natural teeth.2 Depending upon the skeletal relationship of the upper and lower teeth, the patient’s neuro-muscle memory, or engram, moves the lower jaw forward different distances. Patients with a Class II mandibular relationship move the mandible a great distance; those with a Class III relationship hardly move it; and Class I patients’ mandibular movement distance is moderate.
Based on this premise, Pound’s technique requires that the patient pronounce words with the "F" sound to establish the length and position of the upper six front teeth. Figure 6 and Figure 7 show subtle differences in positions of denture teeth on a trial base used in defining the length of the upper anterior teeth.
To determine a patient’s specific location for the lower front teeth, patients are asked to say words with the "S" sound while wearing the trial base to define tooth positions that allow patients to speak clearly. Table 1 summarizes the relationship between skeletal classification and mandibular movements when patients pronounce the "S" sound. This is a movement that cannot be reproduced with an average simulation of mandibular movement and often does not occur in the Sagittal Plane.
Tooth Size, Shape, and Arrangement
Variations in a patient’s dental ridge form and size, facial shape, lip frame, and lip mobility are considered when selecting prosthetic teeth for each patient. One tooth shape or size does not fit all individuals. Patients’ and advisors’ expectations require consideration of a wide variety of artificial tooth forms to create a naturally appearing and mutually acceptable tooth arrangement for a functional prosthesis. A wide variety of artificial forms are available to choose from available mold guides. SR Phonares (Ivoclar Vivadent, ivoclarvivadent.us) and Candulor (candulor.com) provide mold guides offering a broad variety of shapes and shade choices for patients to select and approve.
Lip Frame and Mobility
The lip frame and lip mobility define a dynamic space unique to each patient. This space is bordered by the upper lip, called the grin line, and the lower lip, called the smile line. Each patient has an individual lip mobility movement not duplicated by a generic computer simulation.
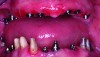
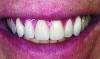
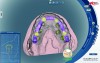
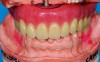
Patients move their lips while smiling and speaking, defining the visibility of the upper and lower teeth when observed outside the mouth. While the occlusal plane is usually defined in relationship to the interpupillary line, sometimes asymmetrical lip mobility heavily influences tooth visibility not defined by bone scaffolding or the occlusal plane. Figure 8 shows the implant distribution, and Figure 9 shows the selected denture teeth on the bite rim. Figure 10 and Figure 11 show the teeth within the lip frame on the trial base while the patient is smiling broadly from the frontal and lateral views. Figure 12 illustrates the completed implant-supported prosthesis.
Perfect Imperfections
While computerized choices may suggest idealized tooth forms and arrangements popularized by the precepts of esthetic dentistry, a more natural appearance can be developed using the concept of "Perfect Imperfections." This concept arranges prosthetic teeth asymmetrically, reflecting individuality using variable tooth shapes and positions.
Perceived personality characteristics related to vigorous or softened appearance apply to the prosthetic principle of dentogenics as suggested by Frush and Fischer.3,4 Dentogenics refers to the philosophy of the prosthodontist replacing lost dentition that reflects the patient’s sex, personality, and age.
Template Development for the Definitive Prosthesis
Completion of the analog complete denture service provides a template used to plan implant placement and design and manufacture a definitive implant-supported prosthetic solution.5,6
Patients often wear the prototype denture prior to implant placement to evaluate function. Once the prototype denture or segmental denture tooth arrangement on a trial base is accepted by the patient, a duplicate prototype upper and lower denture is used during the cone-beam computed tomography scanning process to plan implant placement or scan with a laboratory scanner into the workflow of producing the final prosthesis.
Determination of Space Available for a Prosthetic Device
The vertical dimension of occlusion is an essential factor defined with the prototype complete dentures to assess the vertical space available for a definitive implant-supported prosthetic device during the planning phase of implant placement.
Once all parameters have been addressed with a prototype prosthetic, the developed information is transferred from the analog to the virtual environment and back as part of the planning process for guided implant placement and during the manufacture of the definitive prosthetic design utilizing planning software. Double scanning a prototype complete denture prosthesis and the master impression of the denture ridge with implant abutments in place defines the space available for the definitive prosthetics. Depending on the space available, screw-retained, locator-retained, or cement-retained prostheses are restorative possibilities. This is demonstrated in a scan of the prototype prosthesis superimposed over the scan of the master cast in the planning stages of the definitive prosthetic (Figure 13 through Figure 16).
Use of Prototype Complete Denture as an Interim Prosthesis
The analog prototype denture is often relined and modified during several steps in the implant placement procedures. As a transitional step, it is often attached to the implants at the second stage of the implant-uncovering procedures, acting as a guide to implant abutment options. Once attached to the implants, the converted prosthesis may be utilized to further refine the occlusal and phonetic information to be included in the definitive implant-supported prosthetics.
Conclusion
Ultimately, the manufactured prosthetic must duplicate the information developed within the patient’s individual anatomic situation into the final prosthesis. The final prosthetic placed in the patient’s mouth should provide the comfort, stability, and function that have been the hallmark of conventional processes.
Disclosure
The author had no disclosures to report.
References
1. Brynjolfsson E, McAfee A. The Second Machine Age: Work, Progress, and Prosperity in a Time of Brilliant Technologies. New York, London: W.W. Norton & Co.; 2014.
2. Pound E. Personalized Denture Procedures: Dentists Manual. Anaheim, CA: Denar Corporation; 1973.
3. Frush JP, Fisher RD. How dentogenics interprets the personality factor. J Prosthet Dent. 1956;6(4):441-452.
4. Frush JP, Fisher RD. Dentogenics: its practical application. J Prosthet Dent. 1959;9(6): 914-921.
5. Wade T. Full arch restorations on CAD/CAM-milled titanium bars. Inside Dental Technology. 2011;2(8):46-52.
6. Wade T. Full arch restorations on CAD/CAM-milled titanium bars –part II. Inside Dental Technology. 2012;3(4):2-9.