You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
When presented with larger, more complex cases, the dental team faces a more difficult challenge to control the outcome. Restoring a 3-unit bridge is not a simple restorative case, but it does provide technicians with some parameters. The space being filled is limited by the mesial and distal contact positions and the opposing occlusion. Usually the greatest challenge here is choosing the appropriate restorative material and matching the color, which is typical for most restorative options. The dentist creates a space, and we fill that space. As we evolve in our professions, however, we begin to see that our work is a little more complex than that. Our knowledge of morphology, form, and function are just as critical for the long-term success of the restoration as is our ability to understand the patient’s limitations and expectations from a functional and esthetic perspective. Most important to the success of a restorative case is our understanding of why we are restoring at all. We need to ask ourselves: What was the etiology that created the need for restoration? (Restoring a 3-unit bridge is only easy if we have no knowledge of previous circumstances.) What caused the failure of the natural tooth or the failure of the previous restorations?
Just replacing teeth without knowing the cause for the failure jeopardizes our work. The risk for failure is minimized in small cases in which the limitations of the case will help us achieve success. However, when faced with larger restorative cases, we have a greater risk for failure. A full-mouth reconstructive case can take on a life of its own. First, from a financial perspective, both the dentist and technician may perceive a full-mouth restorative case as a financial windfall. More often than not, in the authors’ experience, this perception falls short of the truth and can sometimes become a greater financial loss than a more simple restorative case. That is because much more diagnostic work and patient communication are involved in the process. In addition, when restoring a full mouth, we must have all the necessary information in regard to the “why” so that we can make the best choices for the “how.” Why is restorative care needed for this patient, and how can we protect our restorations from the same fate in the years to come? In the authors’ experience, esthetics is usually the driving force behind case and treatment acceptance for patients. However, patients are not always aware of their functional attrition. In more extreme cases in which wear has become obvious to the patient, patients are more willing to seek restorative options. They may still perceive the challenge as esthetic based on the wear or discoloration of their teeth that they see. For the dental team, it is critical that we compile all the necessary information in order to aid us in the replacement of what the patient once had and in our ability to give the patient a restorative outcome that once could only be imagined.
Following Functional GuidelinesRegardless of the type of case, when evaluating a patient, esthetic and functional guidelines must be followed. Two considerations must be taken into account.
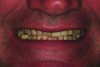
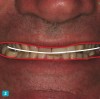
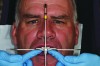
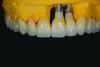
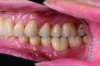
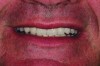
Esthetic and functional parameters: Basically this is where we see the teeth in the patient’s face (Figure 1 and Figure 2). The team’s first esthetic concern is the incisal edge position of the maxillary arch. Understanding the central incisor position and length will help determine the gingival position and alterations if they are needed or will address the gingival architecture.
Occlusal plane: The maxillary occlusal plane is the second parameter of concern. The orientation reference for the maxillary occlusal plane will be based on the horizontal to the floor. Using facial landmarks such as the interpupil line is never recommended. Also the influence of the buccal corridor and the amount of gingival display based on the patient’s facial features, lip dynamics, and age-related parameters can be determined for the patient’s individual esthetics. The lower incisal position and the functional envelope will be addressed only after the maxillary plane has been established. Lastly, the mandibular posterior occlusal plane can be established in relation to the maxillary horizontal and the bilateral support of the posterior occlusion.
Occlusal Concerns
Another challenge in larger restorative cases is understanding the jaw relationship. In smaller cases such as single units and small bridges, we have boundaries to follow and generally work in the maximum intercuspal position (MIP). When the occlusal relationship is failing as a result of tooth wear, migration, chipping, and/or breakage, we can no longer work in the MIP.
To reestablish a proper occlusal relationship, we will need to locate the patient’s centric relation (CR). Unlike MIP, CR is based on the bone relationship with the condyle seated properly in the glenoid fossa. This CR position is a bone-to-bone position and has no relation to tooth contact. Several methods can be used to find the individual CR position based on the practitioner’s expertise and knowledge. The authors recommend using a Kois Deprogrammer. While working in CR, the team has the ability to change the patient’s vertical opening if needed.
Case ReportThe Patient
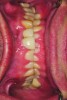
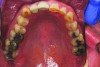
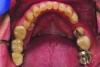
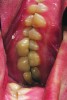
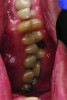
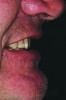
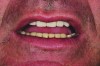
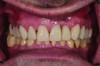
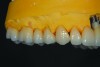
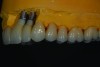
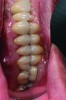
A patient presented with severe loss of tooth structure and several previous subpar restorations (Figure 3 through Figure 8). Following the esthetic and functional parameter guidelines, the incisal position was established. Several methods exist for determining the incisal position such as photographic imaging, a diagnostic wax-up, esthetic transfers, and direct additive. Each technique has value and can be used to secure the proper position. In this case, direct composite was added chairside (Figure 9) to show the patient the potential esthetic changes and to establish a line of communication for the dental team to explain the esthetic direction of the case. Functionally, a Kois Deprogrammer was used to locate the CR position, and diagnostic casts were fabricated and transferred to the laboratory with a horizontal plane analyzer (Kois facial plane analyzer) for mounting (Figure 10). Although the case was mounted on a standard semi-adjustable articulator, we currently have the ability to utilize CAD/CAM for our restorative options. This technology previously worked best for designing and milling substructures but has evolved to allow us to transfer our occlusal parameters and instruments into the CAD software.
The dentist and technician discussed where the incisal edge belonged in the patient’s mouth. Then, a diagnostic wax-up was fabricated following the esthetic guidelines. This lengthened the incisal position approximately 3 mm based on the facial features. The posterior plane was then established based on the horizontal plane and the deficit in the patient’s buccal corridor. Once it was established, the vertical was opened to create the functional parameters.
Preparation guides and a putty matrix were used to prepare the teeth and fabricate chairside provisionals at the new occlusal vertical dimension (OVD). The provisionals were based on the wax-up, and the wax-up was merely the vision of what we believed would be the patient’s esthetic expectations. The authors tested this theory with their first provisionals and anticipated the possibility of alterations to the prototypes based on the patient’s reaction and input. If needed, the dentist can make adjustments intraorally or, in extreme situations, the technician will need to refabricate or adjust the wax-up based on the new information. Once the provisionals had been established, a new study cast and facebow were able to be taken and mounted. This new provisional study cast would be evaluated along with the patient’s photographic information (Figure 11 and Figure 12).
Restorative
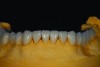
As with all restorative materials, the evolution of zirconia products has produced great esthetic results. Although the use of zirconia for esthetic cases was limited in the past, today’s zirconia structures and layering ceramics are becoming the esthetic choice for a large portion of the restorations fabricated in the laboratory. Zirconia abutments were fabricated on titanium sleeves, and zirconia copings were fabricated with a translucent material. The ceramic layering was completed (Figure 13 through Figure 16), and the final restorations were permanently cemented. A 2-year follow-up showed the patient’s esthetic and functional concerns were met while the occlusal adjustments protected the restorations based on the new functional position (Figure 17 through Figure 21).
Conclusion
To exercise our talents and skills to the fullest potential, we must educate ourselves about the patient’s etiology and use our knowledge of morphology, form, and function to deliver excellent esthetic results.
About the Authors
Jason Bortolussi, DDS, MS, FRCD(c)
Private practice
London, Ontario
Peter Pizzi, MDT, CDT
Owner and Manager
Pizzi Dental Studio Inc.
Staten Island, NY