You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Dentists and dental ceramists provide and sell more than a product. They ask their patients to invest finances and trust in their expertise and skills for performing esthetic dental procedures, as well as the time it takes to complete those procedures knowledgably and predictably.1 As business owners, dentists or ceramists must focus decisions on providing exceptional patient care and choosing the products, services, and systems that maximize their most valuable commodities: time and professional experience.
This can be challenging as new products constantly enter the marketplace and alter patient desires, expectations, and demands, as well as the decisions that dental professionals make.2 More information often is required about the accuracy of available options and their possible implications to the dental care we provide.
Further, with just a “click,” patients can learn about their own role in their dental health and treatment decisions. The digital age has provided dental patients and professionals with an overabundance of information, some correct and some not. But information and technology are not the only requirements for success; processing relevant knowledge from the anecdotal and incorporating it into decisions are also necessary. This requires an inherent human, personal touch, whether purchasing and integrating technology, or applying it to restorative fabrication processes.
For example, because technology is expensive and ever changing, certain factors must be considered for the investment to be successful. These include market trends, uniqueness of the product, what the learning curve is, and marketability to patients— factors that are best analyzed by the people who will be affected by them, not an algorithm.
A humanistic plan for integrating technology will ensure it is embraced for—not dictating or ruling—your patient care. Patients should feel that technology enhances, but does not replace, your personal, professional services. The “personal touch” is an important element of patient satisfaction, and communication and individual skills are key ingredients for esthetic restorative excellence.
This article explains the “personal touch” that dental professionals, whether dentists or ceramists, must apply to several aspects of esthetic restorative cases. These include diagnosis, treatment planning, and communication among all dental team members (eg, dentist, ceramist, patient, specialist). It accounts for the uniquely different perspectives, interpretations, and experiences that affect successful outcomes. Exercising the “personal touch” is also demonstrated in the processes of assessing patient expectations, smile design, provisionalization, material selection, and ultimately fabrication.
Diagnosis and Treatment Planning
Regardless of the type of restorative enhancement, the first human touch occurs during thorough diagnosis and treatment planning. It is here that cooperative interaction between all key players (eg, patient, periodontist, general dentist, prosthodontist, orthodontist, ceramist) should be a priority for treatment, since this interaction ultimately leads to success and greater patient satisfaction.3,4
To facilitate communication among restorative team members, the same set of guidelines and protocols can be used.3 In an ideal situation, the entire team should be able to evaluate the patient during the treatment-planning phase, either in person or by video conferencing. If this is not possible, a very detailed protocol for communication is the next best thing (Table 1).4
Among the facts and pieces of information communicated and shared are clinical and diagnostic data (eg, impressions, radiographs, models, photographs, color tabs). What also must be communicated is the more subjective, “human touch” information regarding what the patient sees as esthetic, since perception of esthetics varies among individuals. While there are guidelines or “esthetic standards” in dentistry, beauty and esthetics are still in the eyes of the beholder.5 Those patient expectations must be clearly defined.
Defining Patient Expectations
Unfortunately, patients use different words in their attempts to communicate, which is why communication takes many turns and twists and can become quite complicated if a standard system to promote mutual understanding is not implemented. For example, what exactly do the words “straight,” “big,” “natural,” “white,” or “small” really mean when a patient uses them? Do they have the same meaning from patient to patient, dentist to dentist, and dental ceramist to dental ceramist?6
The criteria for what constitutes esthetic and artistic perception varies, and multiple external influences affect an individual’s assessment of esthetic treatment needs and choices (eg, type of illuminant, material, perception, professional assessment).7,8 Therefore, involving the patient in the smile design process can be challenging, but it is important for ensuring mutual understanding of expectations and achieving desired outcomes.6
Using communication tools such as a removable, indirect Trial Smile during the pre-treatment stage can help to avoid patient disappointment and enhance communication among team members. With a Trial Smile, not only can patients see and feel their proposed new teeth and their color, shape, and size in their mouth, but it also serves as a blueprint for definitive restorations.6,9
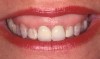
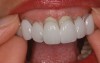
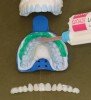
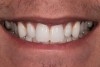
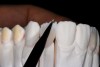
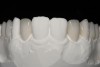
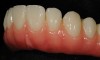
For example, the Trial Smile was useful when restoring a patient who was unhappy with her smile and disliked the old crowns, bonding, and proportions of her teeth, and excess gingival tissue when smiling (Figure 1). To create the Trial Smile, an impression was taken without tooth preparation, and a diagnostic wax up was made. The Trial Smile was fabricated using a cold curing acrylic (Outline, anaxdent, anaxdent.com.com). The patient then was able to place the removable restoration in her mouth (Figure 2), visualize the outcome of the new smile prior to tooth preparation (Figure 3), and share her likes, dislikes, and concerns. This was particularly important because esthetics is very subjective and a matter of personal preference, emotion, and opinion.10
However, it is important that the ceramist fabricating the final ceramics also create the diagnostic wax-up for the Trial Smile and/or the Trial Smile itself. A great number of details must be imparted into these restorations, and esthetic skill and expertise are not merely about a particular product’s or technology’s characteristics or capabilities, but about how the ceramist consistently uses his or her personal touch with the same degree of predictable success, whether the case involves a single crown, multiple crowns, or a combination of veneers, crowns, or zirconia screw-retained implant bridges.1
Understanding Qualifying Differentiators
Whether for Trial Smiles, interim restorations, or definitive ceramics, clinical mastery depends mainly on the expertise of the dental team and the manner in which the selected restorative materials are manipulated in order to realize those collectively understood and communicated patient expectations. Yet, the value of these skills may not be readily apparent to all patients or dentists. Among the reasons for this phenomenon are variations among individuals regarding what they perceive to constitute an esthetic restoration, their ability to discern differences between natural teeth or restorations, differences among their personal preferences, and their brain’s influence in the overall perception of tooth color.10-14 As a result, some patients and dental professionals may believe that a restoration produced digitally, milled, and then customized by a skilled ceramist’s human touch is no different than one fabricated with only a technological process.
It is important to note, however, that as with all forms of art, all ceramists exhibit a different style that is reflected in their interpretation of a dental laboratory prescription or request for a particular type of restoration. If a dentist sends a case with the same instructions to several different laboratories, he or she will receive restorations that demonstrate extremely different appearances because each ceramist interprets the same request with a different vision. This is because artistic and esthetic components of dentistry are subject to perception by the human brain and interpretation by the ceramist’s artistic skills.4,10
Therefore, questions that the restorative dentist should ask when communicating with and deciding upon a laboratory include “Which laboratory’s outcome will satisfy the patient?” and “What kind of tooth preparation will this desired outcome require?” Each laboratory’s vision will require different tooth preparations for space management.
For example, in the case of a patient who disliked her smile and felt her teeth were too short and too yellow, and that the soft tissue lacked symmetry (Figure 4), the ceramist created a wax-up of his vision of the final outcome. This was an extremely important first step to ensure success of the case and allow the patient to better understand the proposed treatment plan.3 The wax-up was created to overlap the soft tissue to lengthen the teeth on the cervical, simulating crown lengthening.
The dentist made an impression of the waxup and then created a mock-up or removable trial smile using acrylic (Luxatemp®, DMG America, dmg-america.com) (Figure 5) and put the direct mock-up Trial Smile in the patient’s mouth (Figure 6). This ensured that the patient would approve of the ceramist’s vision of the final outcome prior to tooth preparation. As with many other cases, waxup and Trial Smile approval formed the basis for dental team communication in the form of surgical guides for the periodontist and preparation guides to ensure enamel preservation and maximized bond strength.
Applying Materials and Technology
Because no single product can resolve the issues of every restorative case, material selection, the ceramist’s skills, and communication are critical to successful case completion. Dentists therefore must be aware of what their selected laboratory is capable of and what their style is. The patient also always should be given options and alternatives, and be made aware of what the possibilities are so that they can make educated decisions.
Skilled ceramists who are now artisans have trained by studying and striving to reproduce natural teeth, with all their diversity, and by learning from their trials and errors.1 We are all striving to create an illusion of reality, and thanks to the newer materials that are available, such as lithium disilicate (eg, IPS e.max®, Ivoclar Vivadent, ivoclarvivadent.com.com) and zirconia (eg, Prettau® Zirconia, Zirkonzahn, zirkonzahn.com.com), this is no longer an impossible task.
Lithium disilicate (IPS e.max) is indicated for numerous restorative applications, including veneers, crowns, inlays, onlays, and implant-supported restorations. For combination cases, it enables fabrication and placement of conservative and “prep-less” restorations, even when altering the appearance of lateral incisors (Figure 7) and blending them with posterior restorations to create a harmonious smile design.
For example, two prep-less lithium disilicate lateral veneers were created with minimal layering to balance the shape of the laterals and blend much more harmoniously with the existing central incisors (Figure 8). Four additional no-preparation monolithic lithium disilicate (IPS e.max) veneers were created for teeth No. 4, No. 5, No. 12, and No. 13 (Figure 9), in addition to a partial monolithic veneer for tooth No. 6. When the type of foundation required is considered for optimal results, the ceramist can apply a human touch to interpret and realize the desired outcome to create a more harmonious smile (Figure 10 through Figure 12).
Certainly, today’s CAD/CAM technology also is enabling advancements in dental restorations, treatments, and communication (eg, simulated smile designs for patient preview; more efficient pre-process restoration design; use of a variety of ceramic, metal, and composite materials).15,16 For example, several sets of provisional restorations can be fabricated from PMMA blocks in exact duplicates (Figure 13). This can enable customization of one set with pink composite for delivery to the patient as an interim, “test drive” provisional (Figure 14), while the other set is used as a more efficient and cost-effective communication transfer tool between dentist and the laboratory (Figure 15).
Further Discussion
Part II of this article, which will appear in a future issue of this journal, will continue to explore the “personal touch” that dental professionals, whether dentists or ceramists, must apply to several aspects of esthetic restorative cases.
Acknowledgements
The author would like to thank the following clinicians for their assistance with these cases: David Garber, DMD (Figures 1-3); Nancy Ray, DDS (Figures 4-6); Marilyn S. Gaylor, DDS (Figures 7-12); and John Heimke, DMD (Figures 13-15).
References
1. Hatai Y. Reproducing nature: understanding the composition of natural dentition. Eur J Esthet Dent. 2008 Winter;3(4):372-80.
2. Culp L, McLaren EA. Lithium disilicate: the restorative material of multiple options. Compend Contin Educ Dent. 2010 Nov-Dec;31(9):716-20, 722, 724-5.
3. Kahng LS. Patient-dentist-technician communication within the dental team: Using a colored treatment plan wax-up. J Esthet Restor Dent. 2006;18(4):185-96.
4. Adar P. Lab talk. Communication: the ultimate in synergy. Inside Dentistry. 2005;1:82-83.
5. Feeley RT. Cosmetics and the esthetic patient and laboratory communication. Oral Health. 1995 Aug; 85(8):9-12, 14.
6. Adar P. Avoiding patient disappointment with trial veneer utilization. J Esthet Dent. 1997;9(6):277-84.
7. Volpato CA, Monteiro S Jr, de Andrada MC, Fredel MC, Petter CO. Optical influence of the type of illuminant, substrates and thickness of ceramic materials. Dent Mater. 2009 Jan; 25(1):87-93. Epub 2008 Jul 7.
8. Tortopidis D, Hatzikyriakos A, Kokoti M, Menexes G, Tsiggos N. Evaluation of the relationship between subjects’ perception and professional assessment of esthetic treatment needs. J Esthet Restor Dent. 2007; 19(3):154-62.
9. Gratton DG, Aquilino SA. Interim restorations. Dent Clin North Am. 2004 Apr;48(2)vii, 487-97.
10. Ahmad I. Synaesthetic restorations: a psychological perspective for surpassing aesthetic dentistry. Pract Proced Aesthet Dent. 2002 Oct; 14(8): 643-9.
11. Haddad HJ, Jakstat HA, Arnetzl G, et al. Does gender and experience influence shade matching quality? J Dent. 2009; 37 Suppl 1:e40-4. Epub 2009 May 22.
12. Mayekar SM. Shades of a color. Illusion or reality? Dent Clin North Am. 2001 Jan;45(1):155-72, vii.
13. Ishikawa-Nagai S, Yoshida A, Sakai M, Kristiansen J, DaSilva JD. Clinical evaluation of perceptibility of color differences between natural teeth and all-ceramic crowns. J Dent. 2009; 37 Suppl 1:e57-63. Epub 2009 Apr 18.
14. Joiner A. Tooth colour: a review of the literature. J Dent. 2004;32 Suppl 1:3-12.
15. Santos GC Jr, Boksman LL, Santos MJ. CAD/CAM technology and esthetic dentistry: a case report. Compend Contin Educ Dent. 2013 Nov-Dec; 34(10):764,766,768.
16. Beuer F, Schweiger J, Edelhoff D, Sorensen JA. Reconstruction of esthetics with a digital approach. Int J Periodontics Restorative Dent. 2011 Apr; 31(2):185-93.
About the Author
Pinhas Adar, MDT, CDT
Adar Dental Network
Oral Design Center, Atlanta
Atlanta, GA USA